The creation of an impactful scenario for clinical simulation requires more than simply gathering equipment and a manikin. It demands a systematic and intentional approach to ensure that the learning experience is both memorable and effective in improving Patient Safety. This process transforms a standard training session into a valuable opportunity for skill development, critical thinking, and teamwork refinement. The goal of this HealthySimulation.com article by contributor Dr. Mario A. Luna Lamas is to provide actionable insights into how to design a highly effective, high-impact healthcare simulation scenario, from defining objectives to running a successful simulation debriefing.
Defining Objectives for Healthcare Simulation Scenarios
The key to unlocking the potential of simulation in healthcare lies in content design that engages the learner, is easy to understand, is immediately applicable, and embodies the spirit of “Edutainment”. With a focus on clear educational goals and real-world clinical challenges, one can guarantee that participants leave the simulation center with skills ready to be implemented. The process outlined here will guide aspiring simulation tech professionals and healthcare educators through the necessary steps to craft scenarios that deliver demonstrable and immediate impact on clinical outcomes.
The foundation of any successful scenario is a set of specific, measurable, achievable, relevant, and time-bound (SMART) objectives. Before the simulation creator writes a single line of the patient’s history, one must determine exactly what skills or behaviors the participants need to master. For example, instead of a vague goal like “improve teamwork,” one could set the objective: “The team will communicate a critical change in the patient’s status using a structured communication tool, such as SBAR, within two minutes of the change being identified”. These objectives directly influence the required level of high-fidelity simulation and the equipment needed. Clear objectives ensure that the scenario remains focused and the post-scenario discussion (simulation debriefing) targets specific learning points. Tools like iRIS can help medical simulation champions write simulation scenarios collaboratively, which can be utilized across multiple modalities such as simulated patients, manikins, task trainers, surgical simulators, wearable simulators and beyond.
View the HealthySimulation.com Webinar How to Implement the Healthcare Simulation Standards of Best Practice Into Your Program to learn more!
Developing the Patient’s History and Scenario Flow
A compelling scenario requires a well-developed patient story that provides the necessary context for the learners to engage. This history should be concise but rich with details relevant to the objectives. One should describe the patient’s background, current symptoms, and any initial actions taken, allowing participants to perform appropriate prebriefing. The flow of the scenario should be structured, typically in stages, where the patient’s condition deteriorates or changes based on the team’s actions (or lack thereof). Careful scripting ensures that the Patient Simulator(s) respond realistically, providing authentic cues to the clinical team. The use of Medical Simulation equipment, such as a Simman or a SimBaby, allows the presenter to introduce expected clinical changes seamlessly, making the experience dynamic and realistic.
Selecting Fidelity and Managing the Pre-Brief
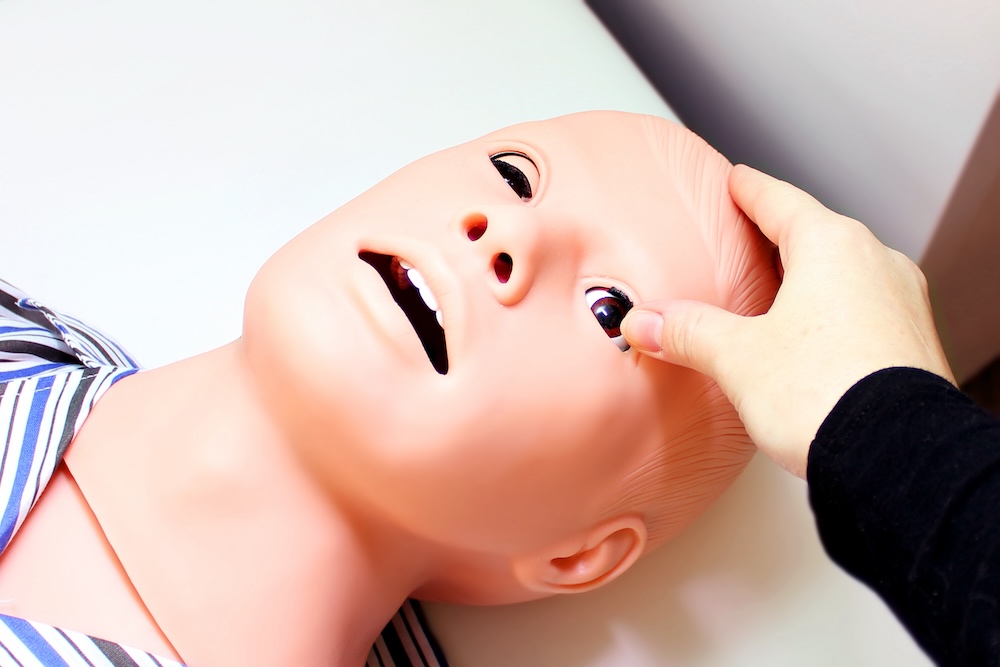
Fidelity refers to the degree to which the simulation mimics reality. Healthcare simulation professionals must remember that high fidelity is not just about the technical sophistication of the manikin. Emotional and environmental fidelity are equally important. One must consider the physical environment, ensure the simulation lab or room is equipped with appropriate medical tools and environmental noise, and create the environment to feel like a genuine emergency room or patient ward. The effective application of moulage to the manikin(s) can significantly boost realism, making physical assessment findings more palpable. When training for high-stakes procedures, such as those that might involve a birth simulator or obstetric simulator, the realism must be carefully managed to maintain a safe learning environment while still achieving the objectives.
Effective scenario execution starts before the simulation begins with a well-delivered prebriefing. The purpose of prebriefing is not to reveal the scenario’s plot but to establish the “fiction contract,” to ensure participants agree to treat the simulation as real. Prebriefing covers logistical information, explains the roles of the sim tech and faculty, and reinforces the core rules of the simulation center, and primarily focuses on a safe environment for learning from mistakes. One must use specifying language to describe the simulation environment as the best way to train clinicians, rather than using the weak and vague pronoun “it”.
View the new HealthySimulation.com Community Scenario Design Group to discuss this topic with your Global Healthcare Simulation peers!
Execute the Clinical Simulation and Manage Situational Awareness
During the scenario, the sim tech operations specialist must manage the technical aspects, which include programming the patient simulators to reflect the clinical changes dictated by the script. The faculty’s role is typically observational, with a focus on documentation of team performance, communication patterns, and demonstration of situational awareness. Situational awareness is important for the participants to maintain a high level in order to interpret all the clinical clues and perform the correct interventions in a timely manner. The sim tech operator must be prepared to make minor adjustments to the script based on participant actions to maintain engagement and clinical relevance. This dynamic management ensures the scenario remains a challenge and focused on the learning outcomes.
The Importance of Healthcare Simulation Debriefing and Feedback
The debriefing is arguably the most critical component of the clinical simulation experience. Debriefing is where the transition from activity to learning truly occurs. The simulation debriefing should be a structured, non-judgmental discussion, typically facilitated by an instructor certified in this area. One should focus on the learners’ perspectives, asking open-ended questions like: “What were your initial thoughts when the patient’s heart rate began to drop?”. This approach allows participants to self-reflect on their performance, identify gaps in knowledge or skills, and reinforce correct actions. The faculty should guide the discussion back to the scenario’s original objectives to ensure the learning outcomes are met.
Technologies like SimCapture from Laerdal, LearningSpace from Elevate Healthcare, SimulationIQ from Education Management Solutions, or other technologies from vendors like KBPort, SIMStation, or Intelligent Video Solutions enable educators to quickly find annotated moments during the video-recorded simulation scenario to playback for learners. Such debriefing systems enables learners to self-reflect through healthcare simulation experiences rather than be lectured by faculty.
Furthermore, once the scenario is complete, one should collect feedback from the participants and the observer-faculty on the scenario’s realism, flow, and effectiveness. This feedback is invaluable for refining future medical simulation programs. For example, if a specific drug is consistently unavailable in the scenario, one might conclude that the inventory system needs improvement in the simulation laboratory. Aspiring Simulation in Healthcare professionals should always look for innovative ways to expand the scope and impact of their scenarios, perhaps by referencing relevant industry standards provided by organizations like INACSL or attending a healthcare simulation conference like IMSH. This commitment to iterative improvement guarantees that the simulation center remains a cutting-edge resource for clinician training.