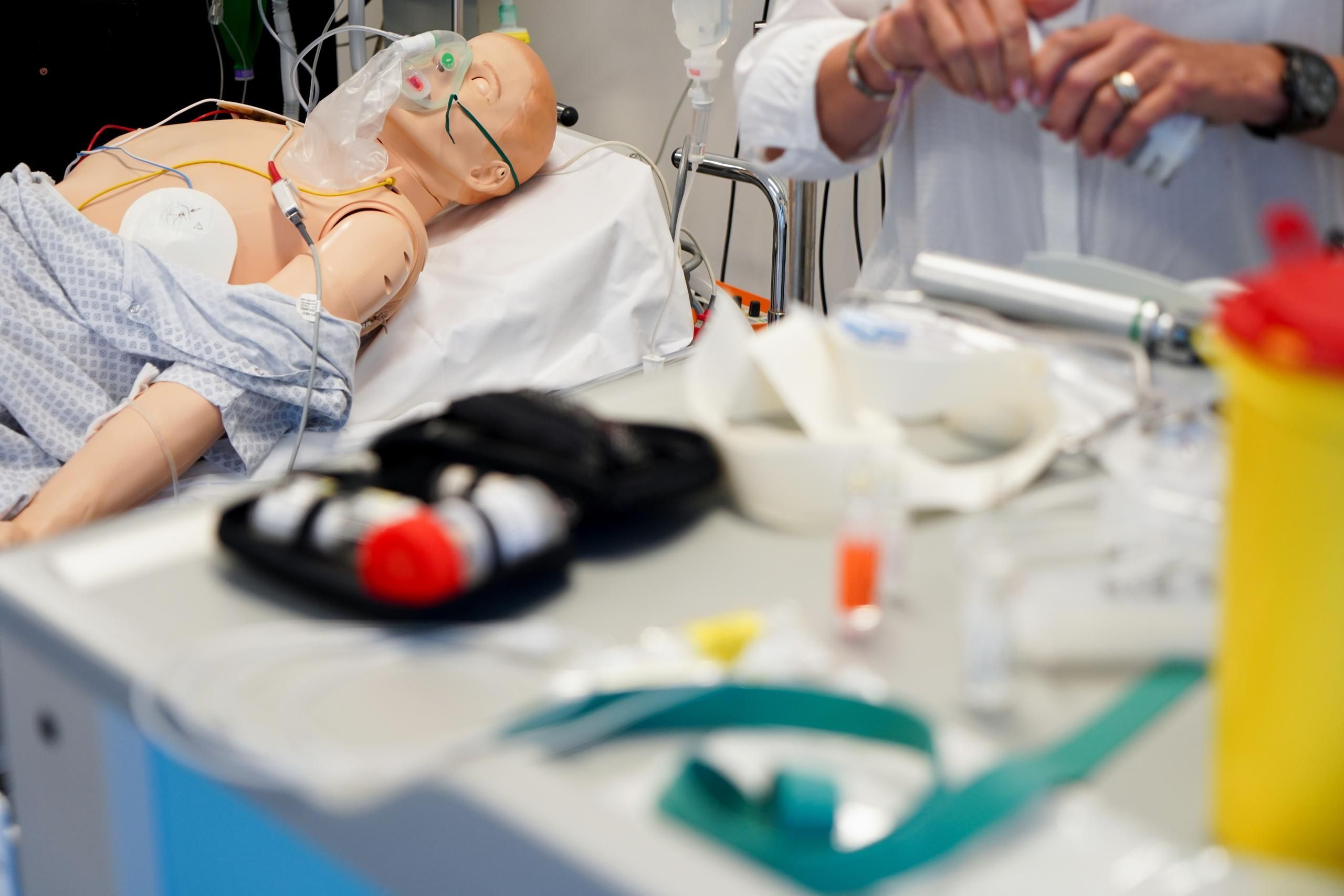
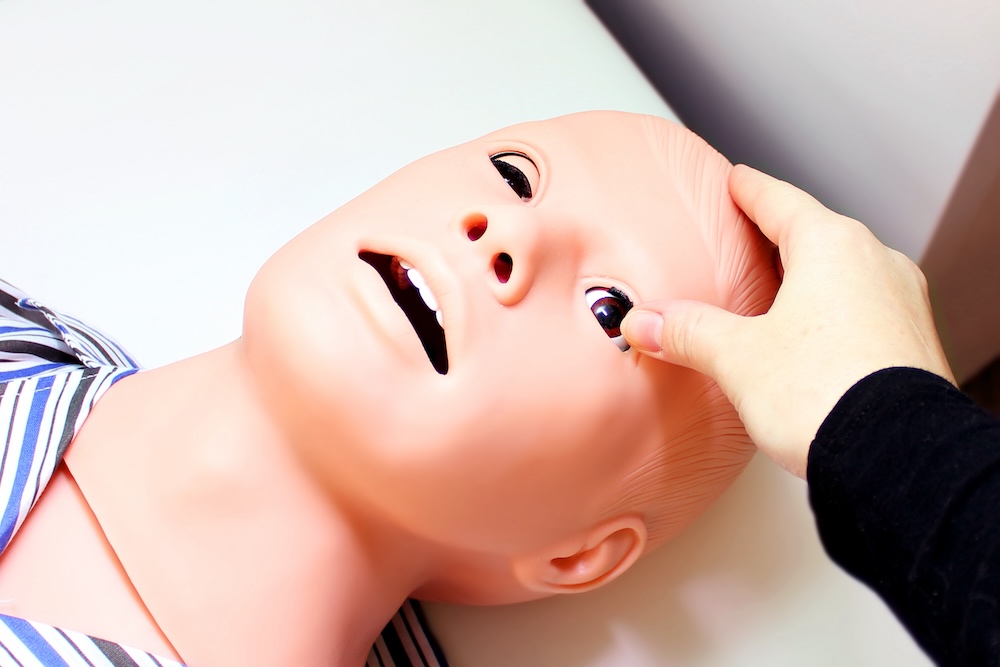
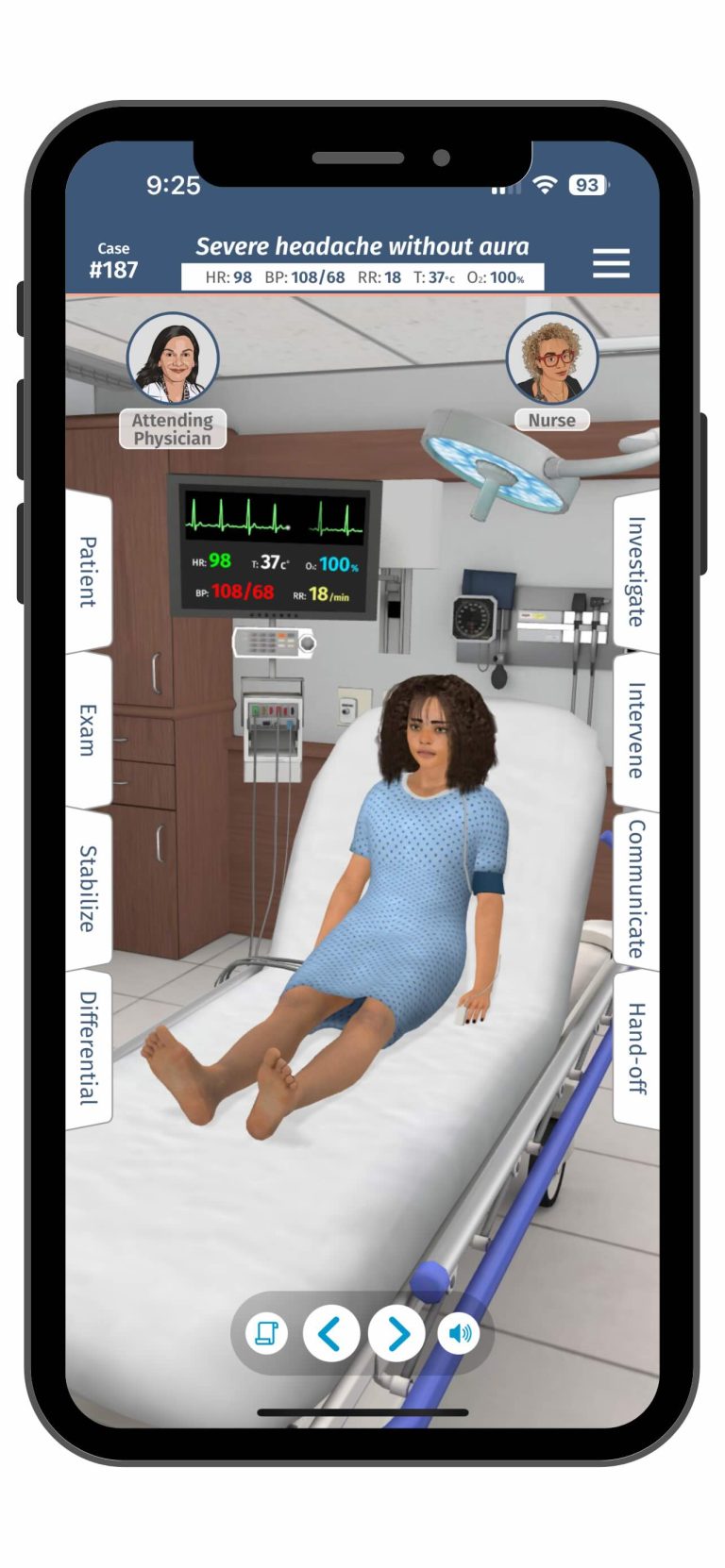
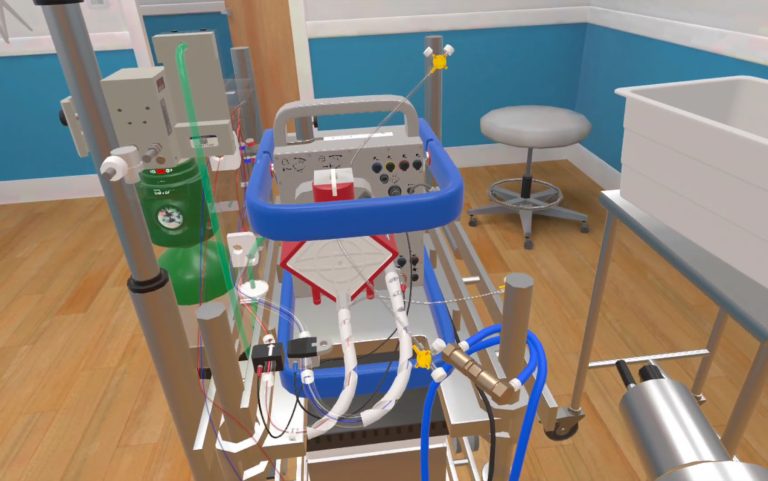
In the world of Emergency Medical Services EMS Simulation, realism reigns supreme. While high-fidelity manikins often steal the spotlight in the chaotic details, the clutter, the background noise, and the unexpected props truly elevate training to reflect real-life field conditions. Healthcare Simulation can do more than replicate vitals and procedures. High-quality healthcare simulation can immerse learners in a fully developed environment that demands critical thinking, quick decision-making, and real-time prioritization. This HealthySimulation.com article by Danny Opperman MBA, NRP, CHSE, CHSOS, Director of Clinical Simulation at the Philadelphia College of Osteopathic Medicine (PCOM), explores how simple props, background manikins, controlled chaos, and ambient noise can increase cognitive load and realism for EMS learners.
Not Just the Patient, Consider the Scene
So, the goal of EMS medical simulation is to make healthcare simulation reflect the real world of emergency medicine: messier, more unpredictable, and ultimately more effective. Healthcare Simulation is theater. And like any memorable production, the power of the scene often lies in the set. Medical Simulation often gets too tidy: one manikin in a squeaky-clean room with all equipment laid out like a surgical Pinterest board. But in EMS Simulation, learners respond to chaotic environments, not sterile ones.
Take, for example, a manikin staged in a public restroom is slumped over a toilet with jeans around the ankles and a tourniquet on the arm; this setup mimics the kind of scene EMS teams routinely face. This would not just be shocking, but instructive, while psychological safety is maintained. This type of scenario immediately sets the tone for urgency and realism, to trigger muscle memory, and scene management skills.
The Unsung Heroes: Background Manikins
If the goal and objective of the EMS simulation is to triage, the educator may want to populate the scene with multiple human patient simulators. This will cause hesitation in a learner’s initial assessment and allow the educator to assess prioritization skills. In one mock waiting room scenario, six manikins sit in chairs: a father holding a baby, a child in a basketball jersey, and an elderly man on oxygen. Are any of them the patient? The learners walked in and froze, unsure where to begin. That moment of uncertainty is golden.
This confusion is the point. In real-world EMS calls, no red arrows point to the correct patient. Scene control and triage begin the moment the provider steps onto the scene. These moments require communication, leadership, and critical decision-making skills. Every healthcare simulation exercise should support the growth of the learners to meet the program outcomes.
Noise: The Invisible But Essential Prop
Sound is an underutilized tool in clinical simulation. Ambient noise disrupts communication, masks patient sounds, and mimics the distractions that EMS teams regularly encounter. The addition of a screaming baby from a Bluetooth speaker behind a couch, the sound of a news anchor on a TV, a fire alarm beeping in the background, or traffic sounds from a city street adds realism to the EMS clinical simulation scenario. These audio layers increase realism without additional cost more than a phone and a playlist.
Use Props Items That Tell a Story
Not every prop needs to function; they can even be broken. Some props simply need to exist, such as: pizza boxes, pill bottles, used syringes, and a tipped-over walker are not junk. These are narrative tools to provide context to the clinical simulation.
Simulation Centers can use these items to drop hints. A collection of empty liquor bottles? Possible intoxication. An overturned wheelchair? Mobility issue or fall. A burned-out toaster next to a bathtub? Electrical trauma or suicide attempt. These details force learners to assess context, not just follow checklists.
Even props, like a manikin with a fake beard, pipe, and glasses, can serve as context clues. This patient may have chronic respiratory issues, or he is a difficult airway case. Maybe, the pipe suggests substance use or exposure to secondhand smoke. The more detail embedded into the manikin’s appearance, the more learners can infer before the hands-on contact with the patient.
View the HealthySimulation.com Webinar Increase Clinical Simulation Knowledge Retention with Scaffolding Cognitive Load Theory to learn more!
Clinical Simulation and Cognitive Load, But with Affordable Realism
The addition of clutter increases cognitive load in a good way. EMS providers must process fragmented, distracting information to make quick, lifesaving choices. When nursing simulation or EMS simulation environments mirror this level of complexity, learners gain practical experience that better prepares them for professional practice.
Simulation labs that mimic disorder prompt learners to scan the room, question assumptions, and reevaluate priorities. These are the same habits that seasoned field providers rely on every day.
This type of immersive simulation in healthcare does not require expensive technology. A broken crutch made from an old mop handle and duct tape creates one scene. While leftover pizza boxes and empty beer cans set another scene. If you have retired manikins that no longer function, they are perfect for set dressing. Simulation labs have the props. They just need to be repurposed. Use those forgotten moulage kits to build the scenario to meet the objectives. What can you do with that mannequin leg in the storage closet? Drape the task trainer over a counter to create the kind of scene that surprises learners and requires creative thinking.
Let the Scene Teach the Case and Practice Unsafe Situations in Safe Spaces
Not every case needs an elaborate script. Sometimes, the healthcare simulation environment tells the story. Picture this: A guy with a majestic beard and a pipe who looked suspiciously like he moonlights as Santa in the off-season. Is it that time of the year already? Or a manikin face-down in a bathtub, a hair dryer floating in water, and a spilled bottle of antidepressants nearby. That’s the script. Learners will generate the questions themselves: “Is this an overdose? Electrical shock? Suicide attempt?” They will start making decisions before any facilitator speaks.
Simulation is the safest place to practice the most unsafe situations. A perfect training room with polished floors and bright lights does not simulate the chaos of a real overdose call. But dim lights, a locked bathroom door, and a moaning manikin behind the door more appropriately sets the scene. Now, that’s a Tuesday night for most EMS crews. The creation of clinical simulation scenarios that feel uncomfortable encourages EMS learners to develop situational awareness and adaptability, key traits in unpredictable field environments.
View the new HealthySimulation.com Community Pre Hospital Simulation Group to discuss this topic with your Global Healthcare Simulation peers!
Final Thoughts: Make Sim Messy, Make Sim Matter
The most effective EMS Simulation scenarios are not tidy. They provide learners with the challenge of a cluttered environment and distractions. That is where the learning happens. Learners can practice scene safety, patient assessment, and situational awareness in a way that prepares them for the unpredictable nature of field response.
Here is a list of common props that every EMS simulation center should have to replicate that classic scene:
- Pack of simulated lighter, cigarettes, cigars, pipe, etc. with ashtray
- Simulated cash
- Simulated weapons
- Simulated iphone/android or flip phone
- Tattoo sleeves
- Simulated food sets (usually child toys/playsets)
- Simulated illegal substances and accessories, etc.
- Tabletop scale
- Pill bottles (make your own labels)
- Extra long nasal cannula that can stretch between rooms
- A wide assortment of clothes, gowns, robes, shoes
- Wigs, beards, hats, etc.
- Glasses, watches, jewelry, rings, etc.
- Wheelchairs, canes, walkers, portable potty
- Simulated feces, urine and blood
- Simulated foul smells in a spray bottle
- Simulated alcohol bottles/energy drinks/milk cartons/soda cans, etc.
- Long-distance Bluetooth speaker that can work in sim space and control room
- Food containers/boxes/tubs, etc.
- Syringes
- Electrical appliances
- Baby toys, bottles, diapers, etc.
- Bluetooth doorbell
- Two-way radio for dispatch/medical control
- Ikea has cheap but reliable furniture
- Standard EMS equipment and supplies
Every detail in a clinical simulation lab tells a story. Every piece of clutter adds a clue. Make learners work for the solutions. The more they have to think, the more they remember. And when the chaos of the real world hits? EMS learners will be ready.