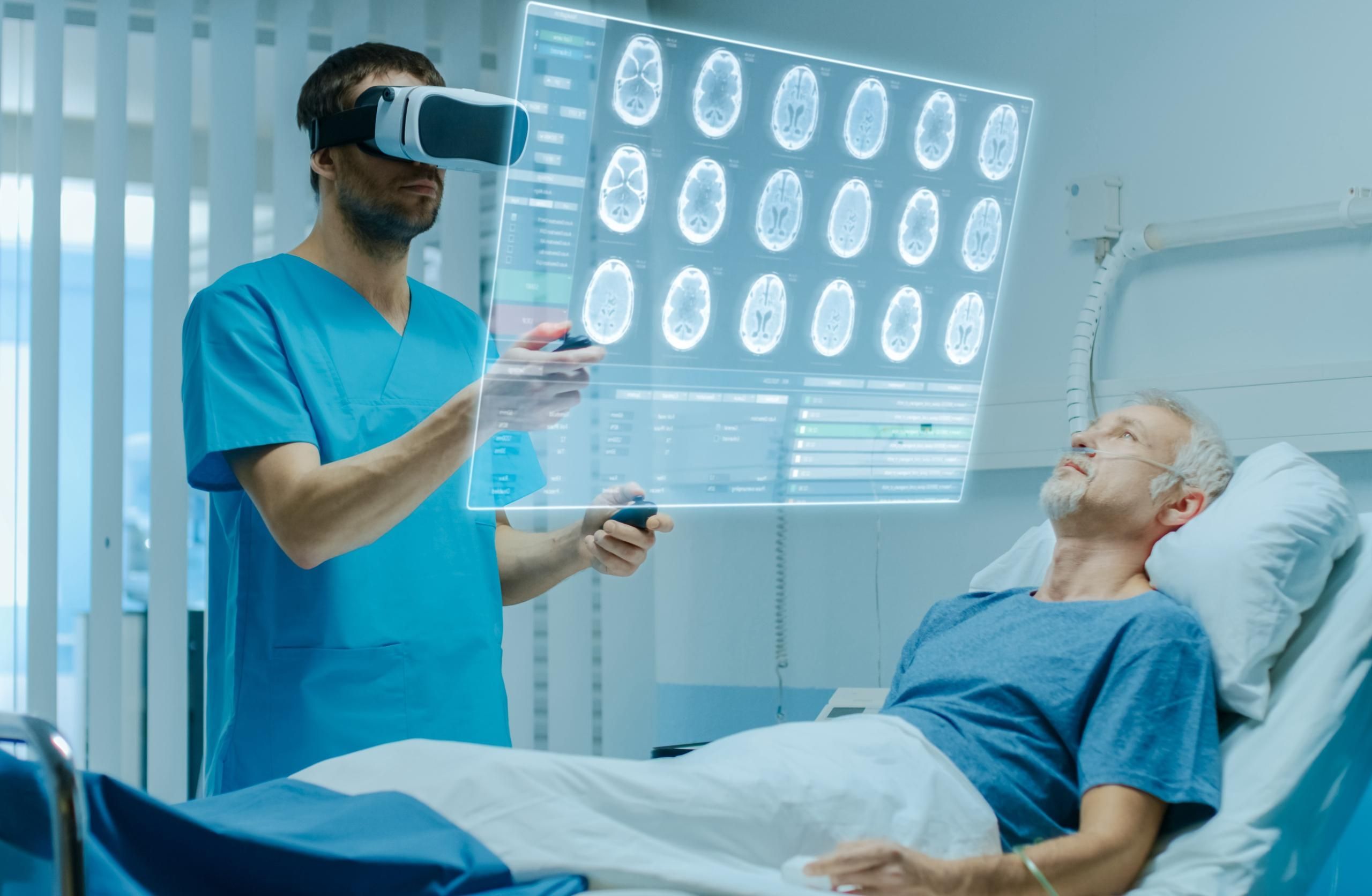
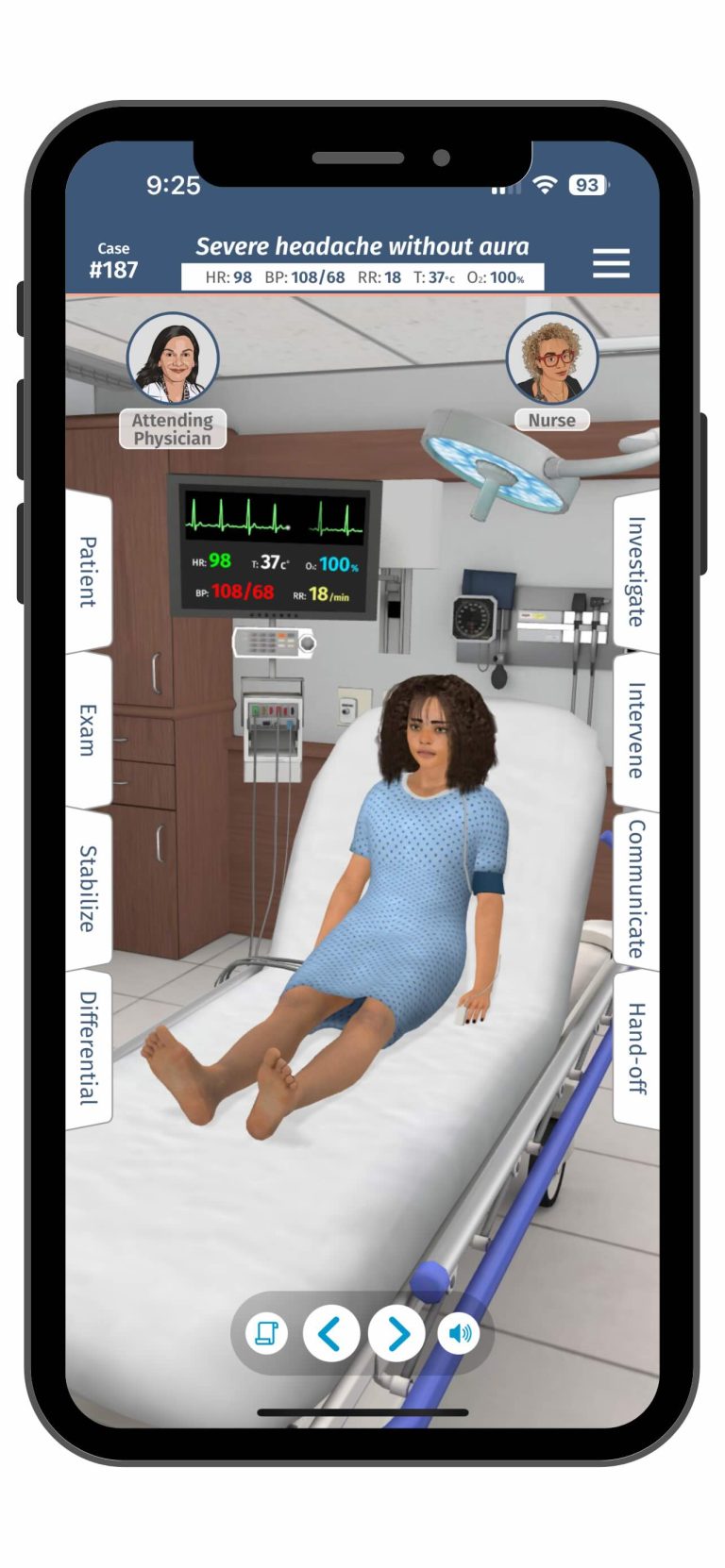
Virtual reality integration has steadily increased in nursing education since COVID-19. The NCSBN study (Hayden, 2014) demonstrated that high-quality nursing simulation, conducted by trained faculty according to healthcare simulation standards, was effective as a substitute for traditional clinical experiences. This landmark study compared traditional clinical experiences with nursing simulation experiences. However, virtual reality was not a standard practice for nursing programs. There has been a gap for in-person and virtual nursing simulations comparison. This article by HealthySimulation.com Content Manager Teresa Gore, PhD, DNP, APRN, FNP-BC, CHSE-A, FSSH, FAAN, is a review of recent studies that compared in-person clinical and virtual reality simulation-based experiences.
Alsharari, A. F., Alrashidi, M., & Alharbi, F. (2025): This systematic review synthesized studies evaluating virtual clinical learning in nursing education. The authors found that VR improved knowledge acquisition, clinical decision-making, and confidence compared to traditional didactic methods. While VR was comparable to other forms of simulation for cognitive skills, it lacked the tactile realism of manikin-based simulation. The review highlighted VR’s scalability and cost-effectiveness but called for more high-quality RCTs focusing on long-term competence outcomes.
Elendu, C., Amaech, D. C., Okatta, A. U., Amaechi, E. C., Elendu, T. C., Ezeh, C. P., & Elendu, I. D. (2024):Simulation-based training (SBT) has evolved from early role-play and rudimentary task trainers to today’s sophisticated high-fidelity manikins, standardized patients, virtual reality platforms, and hybrid simulations, reflecting a steady historical progression in medical education. The authors completed a comprehensive review that traces the trajectory, underscoring how the move from basic skill practice to immersive, technology-enhanced environments has transformed healthcare learning. This historical shift has allowed learners to practice repeatedly in safe, controlled conditions while receiving structured feedback and debriefing, fostering both technical and non-technical competencies. Despite challenges of cost, faculty preparation, and questions about realism, the historical development of SBT highlights its growing recognition as an indispensable strategy for improving patient safety and clinical outcomes, with emerging technologies such as artificial intelligence and advanced virtual reality poised to further shape its future.
Farra, S. L., Gneuhs, M., Hodgson, E., Kawosa, B., Miller, E. T., Hodgson, E., Simon, A., Timm, N., & Hausfeld, J. (2019): This comparative cost analysis examined virtual reality disaster preparedness training versus live simulation drills. Results indicated that while initial VR setup costs were high, VR became more cost-efficient over time as participant numbers increased. Live exercises provided higher realism and psychomotor practice but required greater recurring personnel and material costs. The study underscored the economic advantages of VR for scalable training while acknowledging the enduring need for tactile practice sessions.
Harder, N., Ali, F., Workum, K., Gillman, L., Abdul Rahman, N., & Chiniara, G. (2025): Harder and colleagues explored undergraduate nursing students’ experiences using AI-enhanced VR simulations compared to standardized patient encounters. Students valued VR’s immediate feedback, self-paced practice, and reduced anxiety, while noting SPs offered superior realism for emotional and interpersonal skills. The study concluded that VR is a viable complement to SP training, particularly for building foundational cognitive and communication competencies before higher-stakes, in-person scenarios.
View the HealthySimulation.com Webinar Comparing Standardized Patients vs AI-Enhanced Virtual Patients in Clinical Training to learn more!
INACSL Standards Committee. (2025). Healthcare Simulation Standards of Best Practice®: Facilitation. : This updated Healthcare Simulation Standard of Best Practice emphasizes evidence-based facilitation strategies to optimize learning outcomes across all modalities. It outlines facilitator competencies, learner engagement techniques, and strategies for psychological safety, stressing that facilitation quality drives learning more than modality choice. These guidelines are foundational for both in-person and VR simulation design and delivery.
INACSL Standards Committee. (2025). Healthcare Simulation Standards of Best Practice®: The Debriefing Process. : This standard details the updated debriefing framework, including structured models, facilitator roles, and outcome alignment. It emphasizes that reflective debriefing is a critical determinant of simulation effectiveness, regardless of whether scenarios occur in physical or virtual environments. The standard advocates using structured models such as PEARLS or DASH to improve learning retention and performance transfer.
INACSL Standards Committee. (2021). Healthcare Simulation Standards of Best Practice®: Simulation Design. . The 2021 design standard established a systematic process for designing healthcare simulations, including needs assessment, measurable objectives, fidelity selection, and outcome alignment. It applies to all modalities, underscoring that strong design principles—rather than the medium alone—drive educational effectiveness. The standard remains a cornerstone for ensuring validity and reliability in simulation-based education.
Jiang, N., Zhang, Y., Liang, S., Lyu, X., Chen, S., Huang, X., Hui, P. (2024): This meta-analysis of 27 randomized controlled trials involving 1,480 medical and nursing participants compared virtual simulations (VSs) with mannequins or real patients (RPs) in developing clinical competencies. The findings showed no significant overall differences between VSs and traditional methods in improving knowledge, procedural skills, clinical reasoning, or communication skills, though VSs appeared less effective for nursing participants’ procedural skills and showed a publication year effect on communication skill outcomes. Trial sequential analysis suggested that current evidence remains insufficient, particularly for clinical reasoning. Despite this, the study highlights VSs as flexible, cost-effective alternatives to face-to-face modalities, emphasizing the need for further research on evolving technologies and simulation design features to better inform future medical and nursing education.
Kumar, A., Saudagar, A. K., J., Kumar, A., Yazeed Masaud Alkhrijah, Y, N, & Linesh Raja, L. (2025): This study introduced a low-cost, scalable VR platform for medical education and evaluated its implementation with undergraduate learners. Findings demonstrated significant improvements in knowledge retention and clinical reasoning compared to lecture-based instruction. The authors highlighted the platform’s affordability, ease of deployment, and potential to democratize access to simulation in resource-limited settings, though haptic feedback remained limited.
Liu, K., Zhang, W., Li, W., Wang., T., & Zheng, Y. (2023): Liu et al.’s meta-analysis synthesized randomized controlled trials on VR in nursing education. Results showed moderate-to-large effect sizes for knowledge and skill gains compared to traditional instruction, with no significant difference compared to other simulation methods. The authors noted VR’s high learner engagement and adaptability, but stressed the need for integrating robust debriefing and cognitive load management strategies.
Mitchell, A. A., & Ivimey-Cook, E. R. (2023): This meta-analysis of 59 randomized controlled-trials on technology-enhanced simulation for healthcare professionals. This review indicates that technology-enhanced simulation (T-ES) is effective in improving outcomes across a wide variety of settings and participants. The impact of T-ES was found to be greatest for expert-rated product metrics such as procedural success, and process metrics such as efficiency, compared with knowledge and procedure time metrics. The impacts of T-ES training on the outcome measures included in our study were greatest in nurses, nursing students and resident physicians. T-ES was strongest in studies featuring physical high-fidelity mannequins or centers, compared with VR sensory environment T-ES, though there was considerable uncertainty in all statistical analyses. Further high-quality studies are required to assess direct effects of simulation training on patient and public health outcomes.It concluded that simulation—whether in-person or virtual—consistently improved learner outcomes versus traditional methods. However, evidence directly comparing VR and manikin simulation was limited and heterogeneous. The authors urged future research on long-term transfer to clinical practice and on cost-effectiveness analyses for large-scale implementation.
View the new HealthySimulation.com Community XR – Extended Reality Group to discuss this topic with your Global Healthcare Simulation peers!
Ropponen, P., Tomietto, M., Pramila-Savukoski, S., Kuivila, H., Koskenranta, M., Liaw, S. Y., Mikkonen, K. (2025): Ropponen et al. conducted a meta-analysis examining the effects of VR simulation on nursing students’ competence. They found significant improvements in clinical reasoning, procedural accuracy, and self-efficacy, with pooled results showing equivalence to manikin-based simulation for nursing students. However, most studies had short follow-up periods, limiting conclusions about retention and transfer. The authors advocated hybrid models combining VR with tactile practice.
Sung, H., Kim, M., Park, J., Shin, N., & Han, Y. (2024):This systematic review and meta-analysis assessed the effectiveness of VR in healthcare education across professions. VR showed significant benefits for knowledge, skill, and confidence outcomes compared to non-simulation methods, and performed comparably to traditional simulation. The authors cautioned that high sensory load could impair learning if not scaffolded appropriately, highlighting the importance of design quality in VR implementations.
Talan, J., Forster, M., Joseph, L. &, Pradhan, D. (2025): The authors conducted a qualitative study using semistructured interviews with early adopters of immersive VR simulation technology to investigate use and motivations behind using this technology in educational practice, and to identify the educational needs that this technology can address. Sixteen interviews with VR early adopters. Data were analyzed via directed content analysis through the lens of the Unified Theory of Acceptance and Use of Technology. The main themes that emerged included focus on cognitive skills, access to education, resource investment, and balancing immersion. These findings help to clarify the intended role of VR simulation in health professions education. Based on our data, we synthesized a set of research questions that may help define best practices for future VR development and implementation.
Tong, L. K., Li, Y. Y., Au, M. L., Ng, W. I., Wang, S. C., Liu, Y., Shen, Y., Zhong, L., & Qui, X. (2024): Tong and colleagues conducted research on 270 nursing students randomized into four groups: high-fidelity, computer-based simulation, high-fidelity simulation with computer-based simulation group, and a case study group. Nursing students benefit equally from four methods in cultivating their knowledge, interprofessional collaboration, critical thinking, caring, and interest in learning both immediately and over time. High-fidelity simulation and high-fidelity simulation combined with computer-based simulation improve skill more effectively than computer-based simulation in the short term. Nursing educators can select the most suitable teaching method to achieve the intended learning outcomes depending on the specific circumstances. The authors highlighted the need for validated assessment tools to measure learning outcomes across modalities.
Renee C. Willett, R. C., Ralston, B. H., Martinez-Herrada, A., Chang, T., & Yurasek, G. (2025): While high-fidelity mannequins are effective, they are resource-intensive. Virtual reality (VR) offers a more accessible, immersive alternative. This study compared VR to mannequin-based simulations across four critical pediatric CICU scenarios. Results showed no significant difference in performance: fellows completed similar critical actions and scored an average of 87% on knowledge tests. Participants described VR as more immersive, though some reported mild nausea. This research suggests VR is a promising tool in medical education, offering a realistic and scalable option for pediatric ICU training. Future studies will explore its impact on long-term learning.