The first month of 2026 has proven to be a watershed moment for healthcare simulation research. As educational institutions and hospital systems continue to navigate the post-digital transformation of medical training, the literature published in January 2026 reflects a distinct maturation of the field. No longer are researchers simply asking *if* technology works; they are now deeply investigating *how* it compares to traditional methods economically and pedagogically, and how it can be integrated into complex clinical environments. This HealthySimulation.com article by Dr. Teresa Gore provides a summary of published research studies in healthcare simulation. The topics include integration of Artificial Intelligence (AI) and Virtual Reality (VR), the economic and operational refinement of assessment tools, and the advancement of specialized clinical and surgical skills. View research-related articles from the recent past and subscribe to our free newsletter to stay informed!
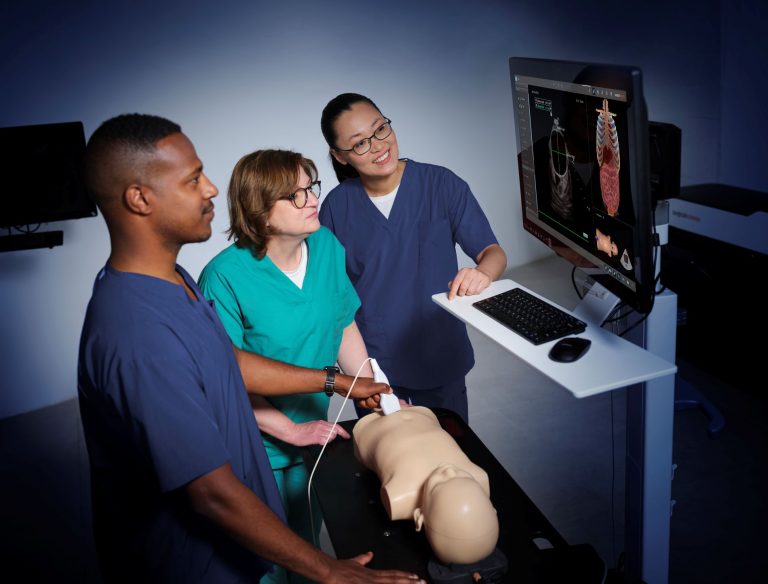
Comparing artificial intelligence-enhanced virtual reality and simulated patient simulations in undergraduate nursing education: This qualitative descriptive study provides critical nuance to the “tech versus human” discussion. The researchers explored the experiences of 240 undergraduate nursing students, with deep-dive qualitative data drawn from 20 third-year students. The findings revealed a complementary dichotomy: while simulated patients (SPs) excel in fostering emotional engagement and hands-on learning, AI-Enhanced Virtual Reality (AI-VR) creates a unique, judgment-free environment that encourages rapid decision-making and iterative practice. The authors conclude that rather than replacing human actors, curriculum designers should adopt an integrated approach that leverages the distinct strengths of both modalities.
Assessing Generative AI Chatbots for Alcohol Misuse Support: Moving from VR to generative AI, a longitudinal simulation study evaluated the efficacy of AI in direct patient support roles. This high-profile research assessed how effective AI chatbots are when tasked with providing support for alcohol misuse, signaling a growing trust in evaluating AI tools through rigorous simulation before clinical deployment.
Cost Analysis of the OSCE: Scoping Review: This timely review addresses the financial burden of high-stakes testing. By analyzing the economic components of Objective Structured Clinical Examinations (OSCEs), the researchers compared traditional face-to-face methods with virtual or hybrid formats. The findings highlight the cost-effectiveness of hybrid and online formats, offering a compelling economic argument for modernizing assessment protocols without sacrificing quality.
Simulation Operations Needs Assessment Tool: : This article details the creation of a new instrument designed to evaluate the operational needs of simulation programs. The study provides validity evidence for the tool’s use in professional practice, filling a gap for administrators who need data-driven methods to justify resource allocation and program expansion. A copy of the SONAT tool is available on HealthySimulation.com.
View the HealthySimulation.com Webinar Assess, Align, Advance with SONAT: New Healthcare Simulation Operations Needs Assessment Tool to learn more!
Novel Simulation with 3D-Printed Spine for Teaching Durotomy Repair: A Technique Guide and Validation Study: This study introduces a novel 3D-printed model specifically designed for surgical trainees practicing the repair of dura mater tears. The findings indicate that this model provides a realistic, risk-free environment that significantly improves the skills of residents, allowing them to practice delicate repairs before entering the operating room.
Mastery Learning Improves Simulated Distal Radius Fracture Management by Emergency Medicine Teaching Faculty: Research appearing in *Simulation in Healthcare*’s publication-ahead-of-print section in January focuses on emergency medicine. The study demonstrates that implementing mastery learning protocols leads to demonstrable improvements in how emergency medicine faculty manage distal radius fractures, reinforcing the value of competency-based education over time-based training.
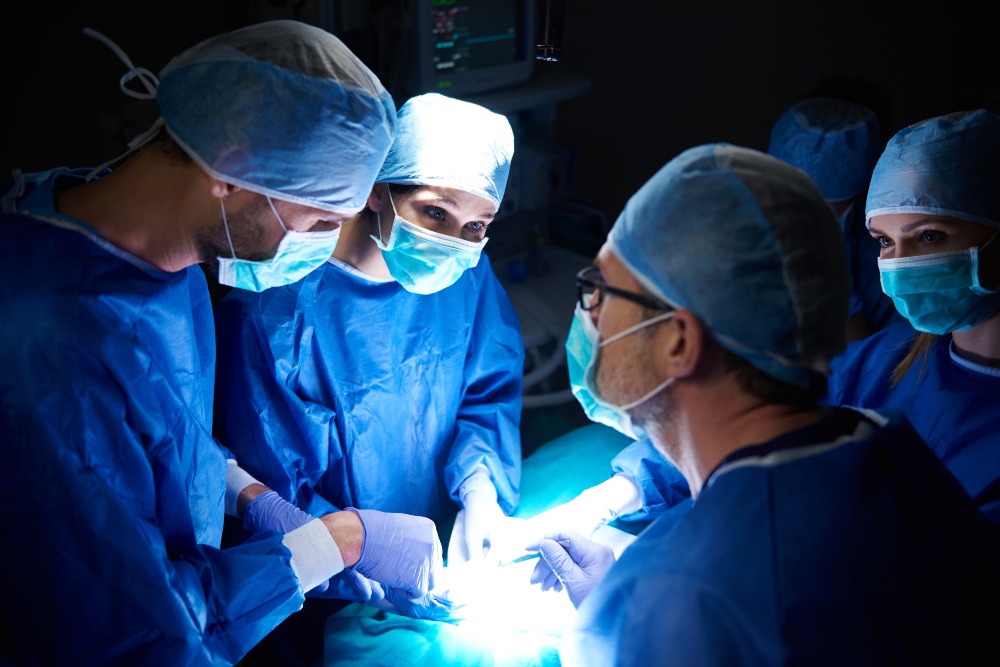
Stress Responses and Experiences of Surgical Trainees in Simulation-based Training of Advanced Laparoscopic Procedures in Highly Realistic Environments: This article investigates the physiological reality of simulation. By monitoring trainees during advanced laparoscopic simulations in highly realistic environments, the researchers provided new insights into the physiological stress responses elicited by simulation, suggesting that high-fidelity environments successfully replicate the pressure of the OR.
View the new HealthySimulation.com Community Simulation Research Group to discuss this topic with your Global Healthcare Simulation peers!
The CHILD Safeguarding Simulation Study: Co-designed Child-centred Interprofessional Learning through Dialogue for healthcare professionals: This co-designed, child-centered interprofessional learning study focused on one of the most difficult conversations in healthcare: child safeguarding. The findings suggest that simulation significantly improves dialogue and collaboration among healthcare professionals regarding the protection of vulnerable children.
Transfer of Clinical Debriefing from Simulation to Practice: A critical look at the “after-action” review, this study by Dewdney et al. explores the barriers and enablers for applying debriefing skills learned in simulation to real-world clinical practice, helping bridge the gap between the sim lab and the ward.
A New Remote Digital Training System to Improve Neonatal Resuscitation Continuing Education Program in Low-Resource Countries: Highlighting the global equity potential of simulation, this study evaluated a distance-learning program using a new telesimulation device. The results were profound, reporting a 71.42% improvement in nontechnical skills among healthcare workers, demonstrating that low-cost, remote simulation can drive massive gains in patient safety in resource-limited settings.
Simulation-Based Education for Extracorporeal Membrane Oxygenation and Strategies for Implementation: A Systematic Scoping Review: Simulation-based education (SBE) in health care is expanding in both scope and relevance. As on-the-job training is challenging in extracorporeal membrane oxygenation (ECMO), SBE is strongly featured in its curricula, yet little is known about its efficacy. Four databases were searched and a narrative synthesis of 28 studies investigating SBE in ECMO was conducted. Notably, there was no standardized SBE ECMO curriculum across studies. Nonetheless, taken together, these articles suggest that simulation improves competency scores, confidence, teamwork, troubleshooting emergencies, and times to critical actions and cannulation. Although SBE reporting in ECMO is heterogeneous, simulation may be comparable to, or even more effective than, conventional training methods. Retention of knowledge and skills over time remains unclear, though regular simulation training may be beneficial. There is a need to establish standardized ECMO curricula that include SBE as a core component.
The research output from January 2026 paints a picture of a field that expands the boundaries of healthcare simulation and education. There is a move toward hybridity, blending AI with human emotion, and the combination of cost-effective virtual assessments with traditional rigor. Simultaneously, the focus has widened to include everything from global telesimulation initiatives to the precise physiological monitoring of surgical trainees. For educators and practitioners, the message from this month’s literature is clear: successful simulation programs must now balance technological innovation with rigorous economic analysis and a deep commitment to human-centered care.