Neonatal simulation-based learning has rapidly emerged as a medical learning strategy, particularly in neonate intensive care, which obviously demands high precision. Neonates are vulnerable populations that require attention and care from skilled healthcare professionals. However, many healthcare workers feel fear and a lack of confidence when they approach a neonatal emergency. A high-fidelity neonatal simulator can provide a realistic training tool to bridge this gap and enhance neonatal care in emergency settings. This HealthySimulation.com article by contributor Bhavesh Patel, MD, explores how neonatal simulators can be helpful in paediatric training programs to improve learners’ skill, accuracy, and competency in neonatal emergencies.
Understand the Learning Gap in Neonatal Emergency Care
Paediatric resident trainees and nursing students often feel nervous during their initial exposure to the delivery room and neonatal ICU. The burden of working with critically ill newborns with unfamiliar procedures and rapid decision-making can lead to errors and burnout. Orthodox learning methods are not enough to prepare healthcare workers for the challenges of neonatal resuscitation. This is where simulation-based learning, especially with a high-fidelity neonatal simulator, plays an important role to provide a controlled and realistic environment for skill development.
Introduction to High-Fidelity Neonatal Simulators
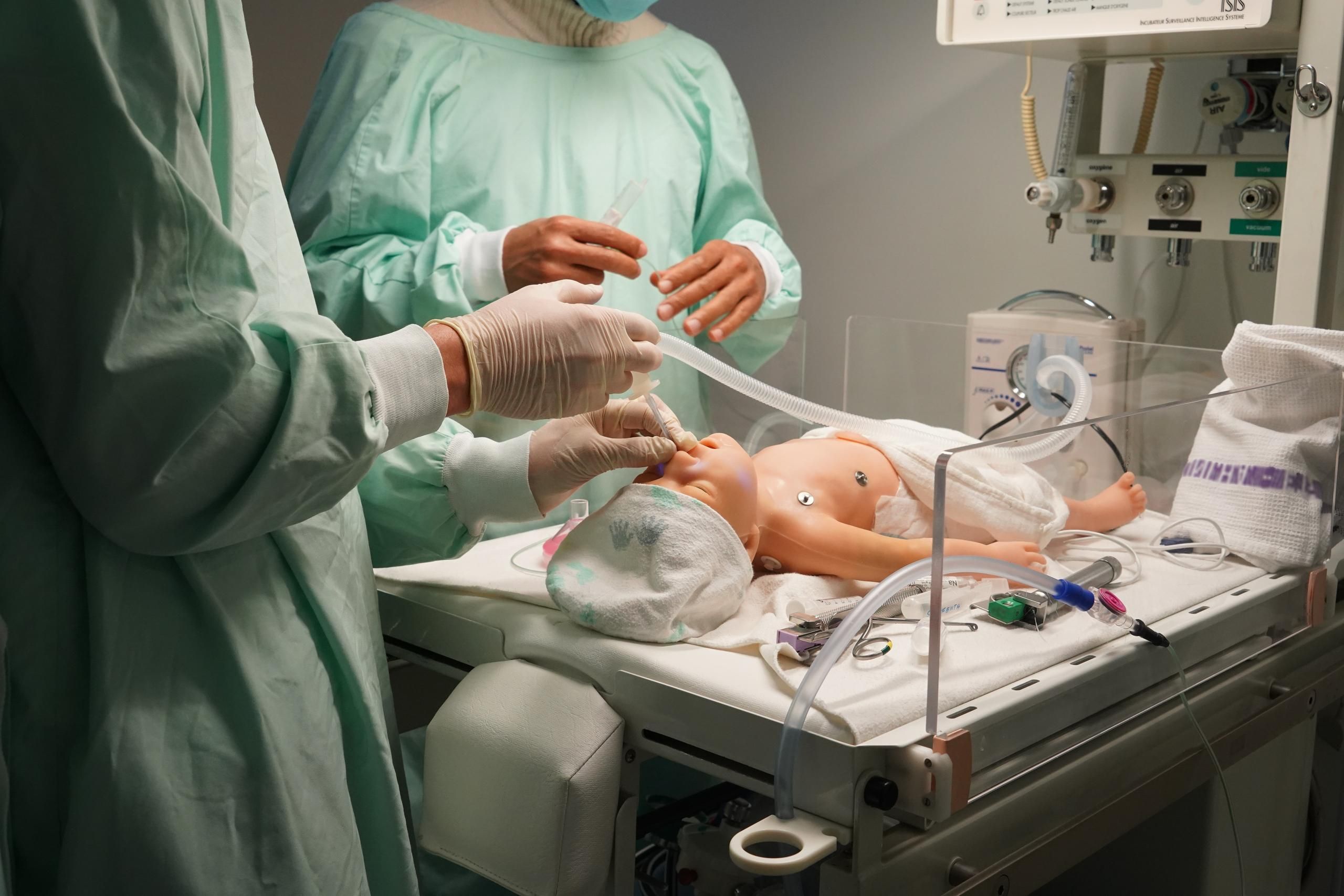
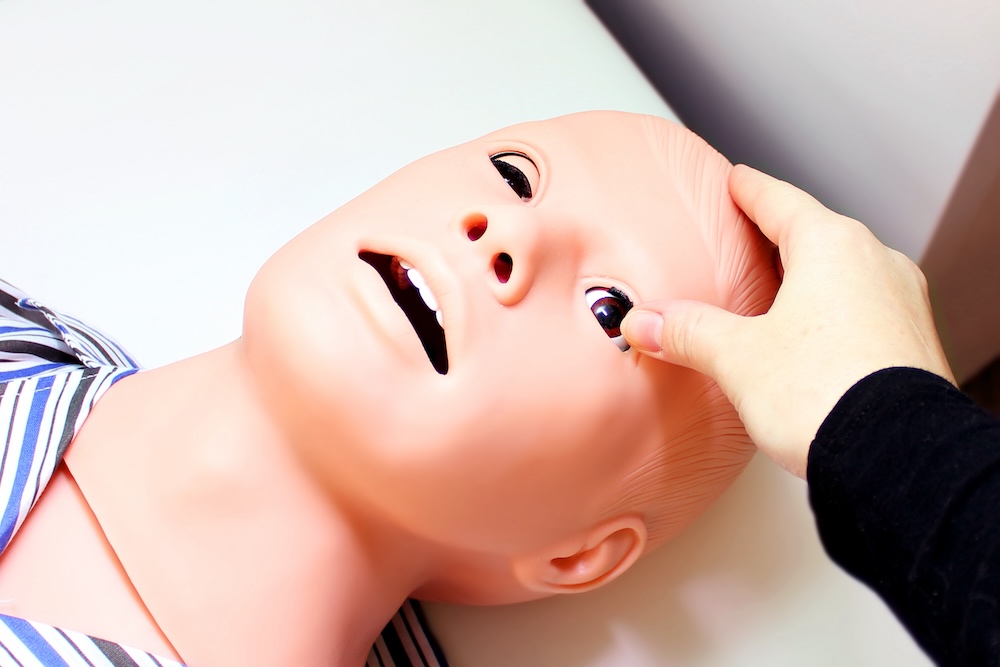
A high-fidelity neonatal simulator can mimic real-life patient responses in a controlled environment. A basic neonatal manikin gives access to basic skills like CPR or ventilation. This lacks many features that high-fidelity neonatal simulators offer. The high-fidelity neonatal simulator is designed with realistic neonatal skin, body weight, and body movements similar to a newborn. The high-fidelity neonatal manikin includes features like normal limb movement with normal or abnormal tone or seizure activity. These high-fidelity manikins can generate spontaneous respiration with chest rise or laboured breathing. Pulse can be palpable at different locations, like the carotid or femoral. Certain areas have variable skin colour that can mimic cyanosis, pallor, or icterus. While practicing an emergency scenario, a learner can have IV, IO, or umbilical catheterization access. Some of these simulators have simulated ECG pads and monitors to observe BP, SPO2, or respiratory rate. Wireless control and pre-installed scenarios that can give learners a realistic feel.
View the HealthySimulation.com Webinar Assessing Team Performance in Simulated Neonatal Resuscitation Programs to learn more!
Neonatal simulators are available from companies such as SIMCharacters (recently acquired by Laerdal Medical), NeoSim AG, Medical-X, Gaumard, Elevate Healthcare, and other global healthcare simulation manufacturing vendors.
Pre-briefing and Orientation of the Neonatal Simulator to Reduce Anxiety
Learners should be given an orientation about the features, functionality, and usage of the simulator. This orientation can be done by verbal introduction at the beginning of training. A slide presentation with a step-by-step protocol for resuscitation can also be used. Video presentation can also be used to reduce the fear and hesitation of first-line learners.
Simulation-based Learning for Neonates
Neonatal simulators can generate real-life emergency scenarios. A pre-installed or custom-built scenario provides the learner access to present challenges.
- Initial process of newborn birth and normal delivery
- Initial scenario of neonatal resuscitation
- Birth asphyxia or respiratory distress
- Neonatal seizures
- Neonatal jaundice or cyanosis
- Teamwork and advanced steps
Skill Station Training – Train for Skills Without the IPE
A neonatal simulator can be used for individual task training to master the psychomotor skills before engagement in the full scenario.
- Initial steps like dry, warm, or stimulate the newborn
- Airway management—mask position and proper seal, bag and mask ventilation and rhythm or rate of BMV, intubation procedure and rhythm and rate
- Chest compression training
- Identification of scenario-based or vital cries, body movement, and respiration.
- Infusion of intravenous medications with IV, IO, or umbilical access.
- ICD insertion for pneumothorax
- Post-resuscitation protocol
A Multidisciplinary Approach
A realistic scenario in a neonatal emergency can have communication errors and overlapping procedures between two departments. Unclear roles between two care providers can impact the outcome. A delayed response in an acute emergency can lead to failure of resuscitation. Sometimes, even highly skilled healthcare workers fail when they have poor communication or inadequate mental preparedness for teamwork. This requires teamwork training with experiential learning exposures.
One task of neonatal ventilation can be carried out by different departments. Paediatric residents take the lead to dry, warm, and manage the airway of neonates. Nursing staff support in equipment availability and documentation. Neonatologists guide throughout complicated situations. The purpose of this teamwork is to practice proper communication and understand the role of each healthcare worker under the recognized leadership.
View the new HealthySimulation.com Community Pediatric Simulation Group to discuss this topic with your Global Healthcare Simulation peers!
Real-time Feedback Provides Immediate Learning
Each step performed by the learner is recorded in a log with timings and the effectiveness of the procedure. After each procedure, the software provides a score for each step. This helps learners and instructors gain insight into common errors while performing procedures and the level of adherence to protocols. The effectiveness of teamwork can also be analyzed to improve communication between different departments.
Psychological Safety and Proven Results of the High-fidelity Neonatal Simulator
During simulation learning, learners can make errors without the risk of harm to actual patients. These mistakes should be viewed as an opportunity for learning. Instructors must establish a culture to build collaborative and adaptive thinking that supports:
- Open-mindedness
- Willingness to retry
- Peer learning
- Support
- Error correction
- Protocol adherence
Proper training with a high-fidelity neonatal simulator improves learners’ neonatal skills test scores. This training increases adherence to resuscitation steps and improves accuracy in real-time crises with reduced fear and stress.
Potential Errors While Learning with a Clinical Simulator
The simulator can mimic a real-time scenario of a neonatal crisis, but may not replicate the exact physiology or pathology in all scenarios. In some scenarios, tone, respiration, or cry cannot be generated exactly like a real newborn. This can lead learners to misjudge certain real-life situations and result in under-resuscitation. The simulator, while applying resuscitation steps, cannot deteriorate unless instructed to do so by the instructor. This may fail to create emotional liability in the learner. Some of the basic steps, like hand hygiene and aseptic precautions, can be missed or overlooked in training unless focus is made on them.
Challenges with the Transition From Patient Simulators to Real Patients
Real scenarios are always unpredictable. Residents should be trained under the observation of a skilled paediatrician for the initial months to be sensitized to all situations. Resuscitators have to face many other challenges apart from sick newborns, like resuscitation failure or emotional parents. Decision-making is the real challenge with a real patient in a critical scenario.
The cost of the medical simulator and accessories is very high. Labs require space and infrastructure that require budgetary support. Training requires skilled instructors who can fully equip learners with the necessary resuscitation skills and protocols. The high-fidelity neonatal simulator is a transformative educational tool for paediatrics and nursing educators. The integration of high-fidelity simulation into the training program is expected to yield a positive outcome.
Learn More About Healthcare Simulation to Promote Teamwork!
References
- Lindhard, M. S., Thim, S., Laursen, H. S., Schram, A. W., Paltved, C., & Henriksen, T. B. (2021). Simulation-based neonatal resuscitation team training: a systematic review. Pediatrics, 147(4).
- Soghier, L. (2024). Improving neonatal patient outcomes using simulation-based education. The Journal of Pediatrics, 266.
- Gray, M. M., Umoren, R. A., Josephsen, J., Chitkara, R., Strand, M., Ramachandran, S., Weiner, G., Zaichkin, J., Sawyer, T., Billimoria, Z., Kristensen Cabrera, A., Motz. P., Sie, L., Weiner, Y., Kan, P., Stavroudis, T., Ades, A., & Lee, H. C. (2020). Gaps in Neonatal Provider Performance on Standardized Simulations: A Report from the NRP eSim™ Study. Pediatrics, 146.