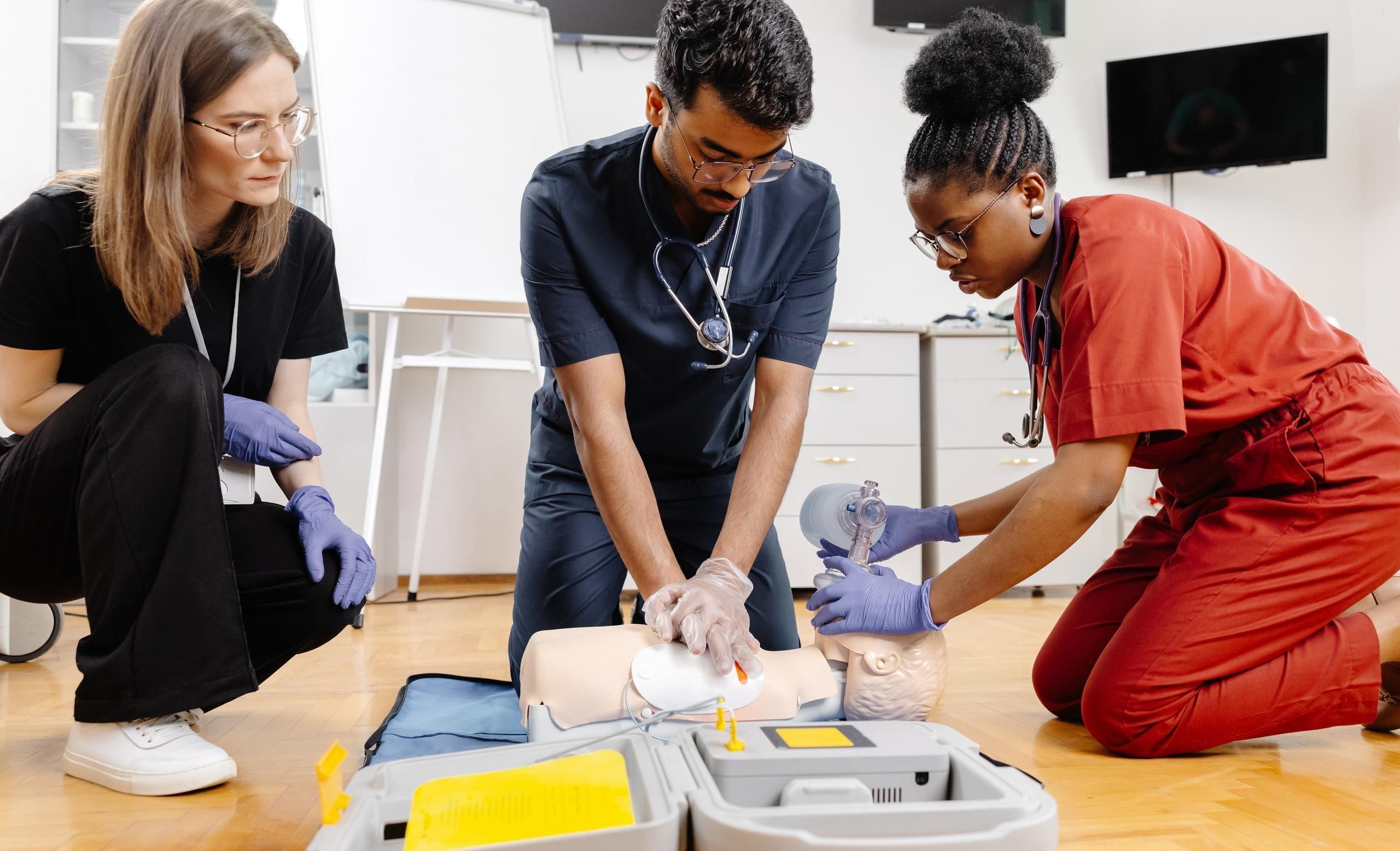
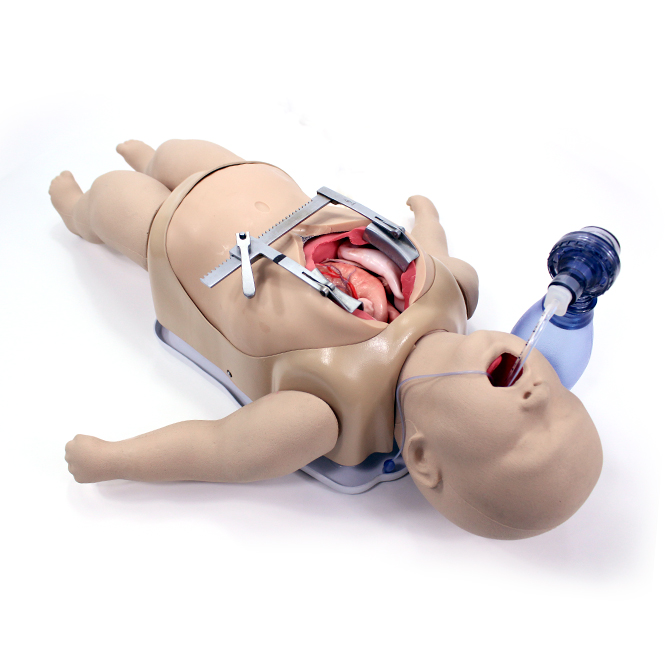
In November 2025, the American Heart Association (AHA) published its major revision of the Guidelines for Cardiopulmonary Resuscitation (CPR) and Emergency Cardiovascular Care (ECC), the 2025 AHA Guidelines for CPR and ECC. These new guidelines have important implications not only for clinicians at the bedside but also for healthcare simulation professionals, simulation operations specialists, and educators who design simulation-based curricula for nursing, medical, and allied health learners. In this HealthySimulation.com article by HealthySimulation.com content team members Dr. Teresa Gore, PhD, DNP, APRN, FNP-BC, CHSE-A, FSSH, FAAN, and Carrie Gigray, MSHS, CHSE, CHSOS, GC-HQS, NRP, the key updates of the 2025 AHA Guidelines are examined with a simulation operations and scenario design focus, and best practices for integrating the guidelines into simulation-based training, lab infrastructure, and assessment are explored.
Major Updates in the 2025 AHA Guidelines
The 2025 Guidelines represent a comprehensive revision across adult, pediatric, and neonatal life support; resuscitation education science; systems of care; and ethics. Some of the key headline changes include:
- Single unified “Chain of Survival” applicable to both in-hospital and out-of-hospital cardiac arrest (IHCA and OHCA), across the age spectrum.
- New emphasis on ‘community initiatives’, lay rescuer training, public access to naloxone (in addition to AEDs), and instructor-led mass training.
- Enhanced recommendations around clinical debriefing (immediate “hot” and delayed “cold” debriefs) after resuscitation events.
- Updated team composition and simulation-training guidance: e.g., in-hospital code teams should include ALS-trained members and dedicated roles, and simulation-based training is explicitly cited as beneficial.
- New ethical content: explicit discussion of structural inequities, distributive justice, provider moral distress, and advanced care planning in resuscitation contexts.
- Strengthened attention to post-cardiac arrest recovery and survivorship, coordinated systems to support functional recovery after resuscitation.
- Neonatal updates: For newborns not needing immediate resuscitation, deferred cord clamping (≥ 60 s), skin-to-skin contact, and updated ventilation/compression algorithms.
- For pediatric patients: minimizing CPR interruptions (< 10 s), closing the gap on older techniques (e.g., the 2-finger infant compressions no longer recommended) and updated foreign-body airway obstruction (FBAO) protocols.
Implications for Simulation Operations
Simulation operations professionals should audit and optimize lab infrastructure to support the updated guidelines and computer-based simulation practice. Ensure manikins, monitors, defibrillators, and simulation programming reflect the updated algorithms (BLS/ALS/NRP) and rescue sequence changes in branching logic. Programming updates to include ETCO2 readings or MAP targets, and a chest compression feedback waveform, can increase fidelity while providing accurate CPR performance metrics. All consumable inventory, such as a pediatric code cart, must have outdated resources replaced with current algorithms, cognitive aids and appropriate equipment (e.g., laryngeal mask, BVM, IV) to support these guideline changes. It may be necessary to procure new training assets and materials, such as LVAD trainers or OB-specific resuscitative kits.
Curriculum Redesign and Scenario Update
Given the number of new and revised recommendations, simulation educators must review and align their existing scenarios with the 2025 Guidelines. Adult Basic Life Support (BLS) and Advanced Life Support (ALS) scenarios should integrate the unified Chain of Survival and community-response links (e.g., telecommunicator guidance, naloxone for opioid overdose). Update PPE requirements to include aerosol-generating procedures for learners should be considered. Pediatric/infant simulations should incorporate updated compression techniques, airway management (as per the new recommendations), and emphasize minimizing pauses. Neonatal scenarios must reflect deferred cord clamping and ventilation strategies, plus team readiness for any birth requiring transition to resuscitation. Team debriefing should be built into simulation workflows: both immediate (hot) debrief at scenario conclusion and a delayed (cold) debrief after reflection/data review. Ethical decision‐making and system-of-care thinking should be embedded into simulation design (for example, scenarios with moral distress, multi-disciplinary team roles, resource constraints).
View the HealthySimulation.com Webinar Rapid Cycle Deliberate Practice: RCDP Simulation for Cardiac Resuscitation Competency to learn more!
Simulation Lab Infrastructure and Management
The 2025 guidelines reinforce the value of event feedback and iterative skills refinement. Healthcare simulation directors should implement Rapid-Cycle Deliberate Practice (RCDP) instructor training to include checklists and pause-point feedback strategies. Support team-based simulation with clearly defined roles, advanced life support-trained operators, and realistic team sizes (as recommended). Integrate debriefing facilities and processes: hot debrief zones (adjacent to simulation bay) and cold debrief / analytics spaces for later review. Data capture and analytics infrastructure: record scenario metrics (compression depth, rate, pauses, ventilation efficacy, team role execution) to align with quality improvement imperatives underlying the guidelines.
Simulation Centers can strengthen long-term sustainability by expanding services to meet updated 2025 AHA community-focused recommendations. The new guidelines emphasize increasing access to opioid overdose education and naloxone administration, along with addressing disparities in CPR training across underserved, low-income, and linguistically isolated populations. Simulation programs can play a central role by offering community courses that include naloxone recognition and response, hands-on overdose training, and culturally tailored CPR education. Through these outreach efforts, Simulation Centers reinforce community readiness, support public health initiatives, and generate revenue streams that sustain high-quality clinical simulation while advancing equitable access to lifesaving skills.
Assessment and Competency Verification
The 2025 Guidelines underscore the importance of high-quality CPR, minimizing interruptions, team composition, and simulation-based training. For simulation educators, this means:
- Competency assessments should include team-based scenarios and metrics aligned with guideline thresholds (e.g., CPR coach, compression quality, pauses < 10 s for pediatrics, correct sequence for FBAO).
- Use simulation-based mastery or deliberate practice models: allow learners to repeat until proficient in the updated techniques (for example, 2-thumb encircling hands for infants).
- Incorporate debrief-driven improvement: use immediate and delayed debriefing to reinforce learning, discuss systemic issues, refine protocols, and foster continuous improvement.
- Link simulation outcomes to real-world system performance: e.g., tracking improvements in lab metrics, pre- and post-implementation of new guideline-aligned scenarios, evidence of improved readiness/rescue quality.
- Integrate new special circumstances to cover high-risk, low-frequency events such as LVAD perfusion assessment and device troubleshooting, hypothermia/hyperthermia protocols or life-threatening asthma refractory emergencies.
- Tie simulation scenarios to system-of-care frameworks: e.g., design scenarios that reflect transitions across the chain of survival, community to hospital, in-hospital systems, and post-arrest recovery with interdisciplinary practice.
Incorporation of Gamification in Resuscitation
Guidelines support the use of gamification technology to improve engagement, spaced repetition, and resuscitation training for healthcare professionals. Virtual Reality (VR) is recommended for knowledge acquisition only and using Augmented Reality (AR) to provide real-time CPR feedback for BLS and healthcare professionals may be beneficial. Healthcare simulation educators and operators should ensure VR modules contain only cognitive content, update algorithms, and replace VR compressions or ventilations with hands-on training using task trainers or manikins. They may also consider the addition of AR in resuscitation scenarios for learners to receive immediate feedback.
Why Healthcare Simulation Matters in the 2025 AHA Guidelines
Simulation has never been more central. The 2025 AHA Guidelines emphasise system-based care, team performance, minimising CPR interruptions, and community response initiatives. These are all areas where simulation excels:
- High-fidelity simulation (HFS) allows teams to practice rare but critical events (e.g., OHCA, pediatric arrests, newborn resuscitation) in a safe, controlled environment.
- Team training and role clarity: simulation can replicate full code team dynamics, role assignments, communication and hand-offs—directly matching guideline recommendations for defined roles and advanced training.
- Debriefing: The guidelines explicitly call for hot + cold debriefing. Simulation offers structured debriefing frameworks (e.g., gather, analyse, summarise) that bring this to life.
- Systems thinking: Beyond individual skill, simulation can model system responses (community to hospital, EMS transport decisions, termination on scene, ECPR centres, etc.) and help operationalize the “systems of care” concept.
- Data capture and improvement cycles: Simulation labs can generate metrics (compression depth, rate, ventilation success, team roles executed) that feed quality improvement loops in line with guidelines emphasis on data review.
- Rapid-Cycle Deliberate Practice (RCDP): Allows learners to increase performance by exposure to multiple rounds of skills with direct feedback at pausepoints or based on actions, often increasing in complexity.
View the new HealthySimulation.com Community Simulation Research Group to discuss this topic with your Global Healthcare Simulation peers!
In short, simulation operations specialists and educators are key enablers of guideline translation into practice. Aligning with the 2025 AHA Guidelines, simulation programmes help bridge the gap between evidence and competence, training and performance, systems and outcomes. Action steps for simulation-based teams for simulation operations and education teams to capitalise on the 2025 guideline update:
- Guideline audit: Review your current simulation catalogue (BLS/ALS/NRP/pediatric/OB/neonatal) and map scenario elements to the 2025 changes (compression techniques, team composition, deferred cord clamping, naloxone protocols, etc.).
- Curriculum update: Revise scenario scripts, learning objectives, debriefing guides, team checklists, and assessment tools to reflect the new recommendations.
- Lab infrastructure refresh: Verify manikin programming (adult, pediatric, neonatal), AED/defibrillator simulation, real-time metrics capture, debriefing rooms, video capture, and analytics dashboards.
- Educator development: Provide “train-the-trainer” updates to simulation educators and instructors on the 2025 guideline changes—especially team training, ethical frameworks, RCPD and simulation-based debriefing modalities.
- Debriefing practice: Build hot (immediate) and cold (delayed) debrief processes into every simulation event. Ensure you schedule the cold debrief separately, review data logs, allow reflective learning, and provide feedback for system improvement.
- Team-based simulation and Assessment: Increase emphasis on full team simulations (in-hospital code teams, community/rescue team links, post-arrest recovery teams). Use metrics to assess performance and provide remediation/practice cycles.
- System integration: Use simulation to test and refine system-of-care links: early warning systems, rapid response teams, community lay-rescuer training programmes, ECPR pathways, post-arrest recovery planning.
- Quality improvement loop: Capture simulation performance data, compare pre/post guideline-aligned changes, feed outcomes into institutional quality improvement committees, simulation governance, and align with accreditation/simulation standards (e.g., INACSL, CHSOS/CHSE domains).
Significant Advancement in Resuscitation Guidelines
The 2025 AHA Guidelines for CPR & ECC mark a significant advancement in resuscitation science and systems of care—and they spotlight the critical role of simulation in turning guidelines into actual performance. For simulation operations specialists and education teams, this means updating curricula, realigning scenario design, strengthening infrastructure, embedding structured debriefings, capturing data, and reinforcing system-of-care thinking. By proactively integrating these changes, your simulation programmes will be better positioned to support clinical teams, improve resuscitation outcomes, and align with emerging best practices in resuscitation education.
As you design your next round of simulation scenarios, ask: Does this reflect the 2025 AHA guideline change? Are my teams prepared? Are my systems designed to measure and improve? Embracing the guidelines through simulation is not just about ticking the box—it’s about elevating readiness, performance, and ultimately patient survival.
Learn More About CPR Manikins from Our Vendor Directory!
References
- American Heart Association. (2025). Highlights of the 2025 AHA Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Retrieved from [ https://cpr.heart.org/-/media/CPR-Files/2025-documents-for-cpr-heart-edits-posting/Resuscitation-Science/252500_Hghlghts_2025ECCGuidelines.pdf]