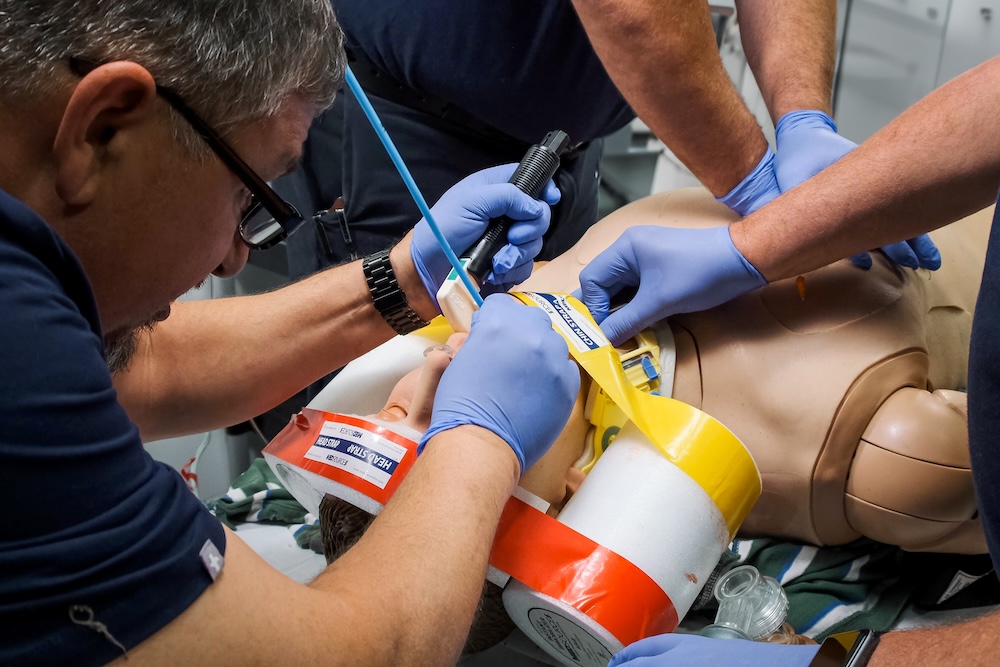
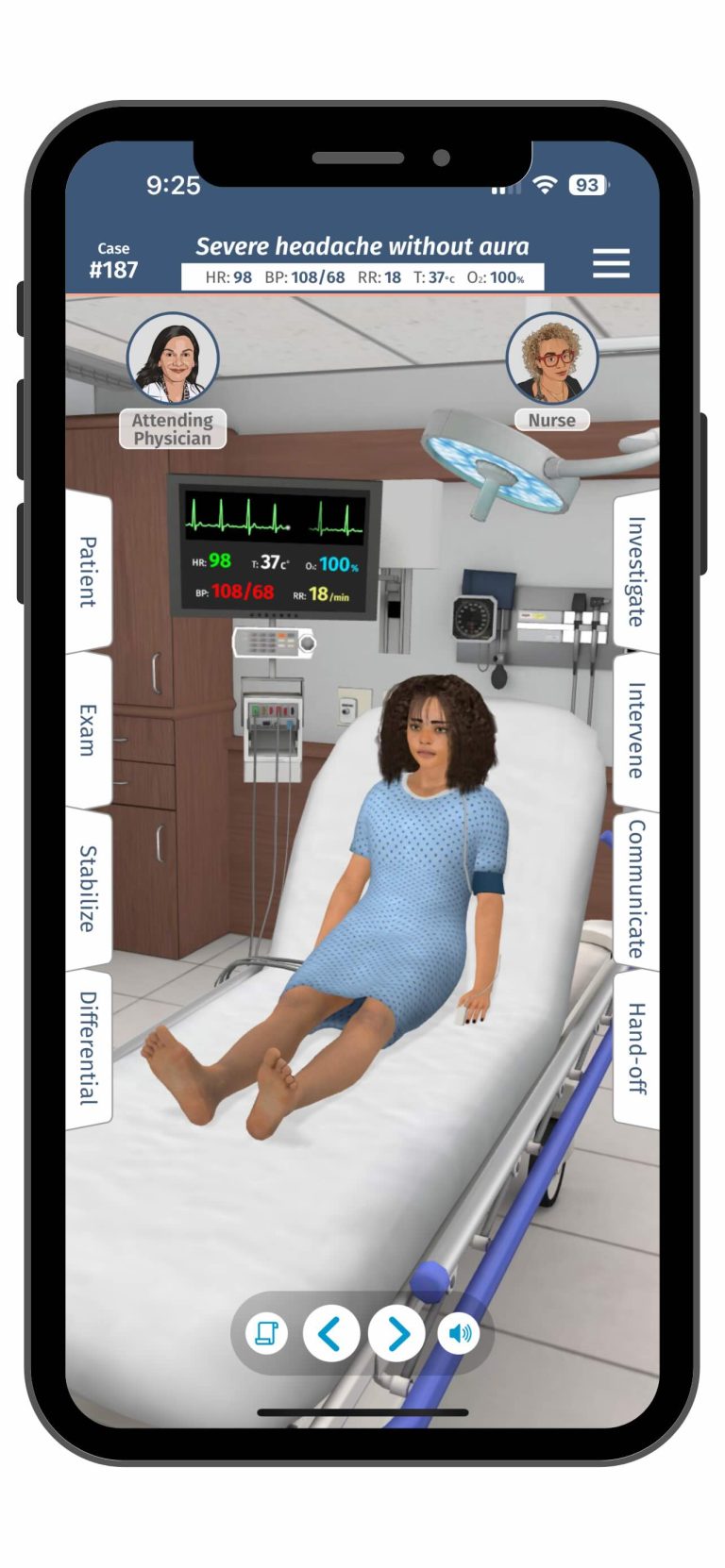
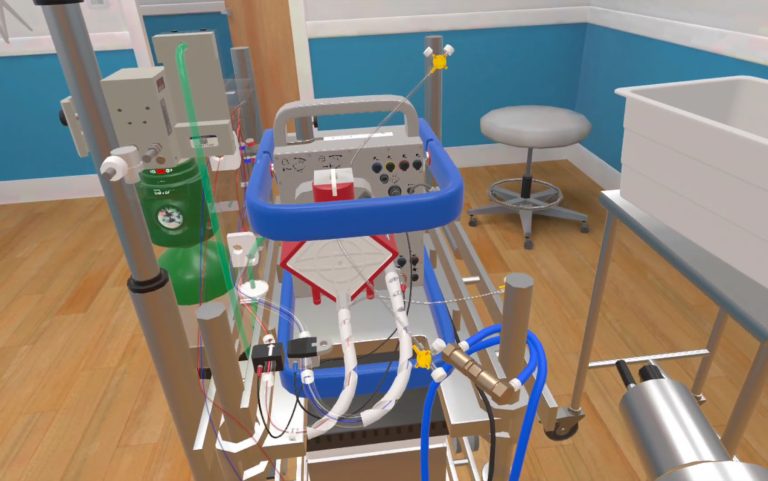
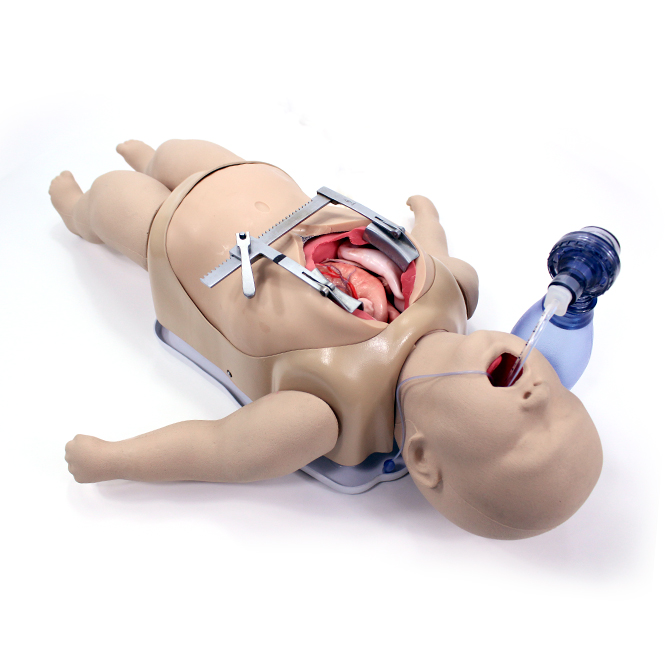
On a regular day, most simulation centers operate as a well-structured environment. The day-to-day work is carefully planned: courses are scheduled weeks or months in advance, scenarios are meticulously written and rehearsed, instructors are trained and assigned specific roles, and every piece of equipment is calculated and checked before a session. Teams have the time and resources to create immersive environments, develop high-quality moulage, and conduct thorough debriefings with full audiovisual support. This predictable structure ensures a smooth workflow and consistently high learning outcomes. However, with the recent episodes of mass casualty events worldwide, simulation centers are required to help train hundreds of medical professionals to provide trauma care rapidly. This HealthySimulation.com article by Ella Ehrenfeld, MSN, B.EMS, RN, Head of Medical Simulation Center in Israel, will explore a step-by-step process to address how to build a mobile, scalable medical simulation training system for emergency situations.
World Events That Require Mass Casualty Care
Areas or regions of the world can change overnight. When an emergency event, such as a massive earthquake, flood, or war, occurs, healthcare professionals must shift their specialty care focus and respond to meet the public’s needs. Healthcare simulation can help with this transition. Healthcare simulation programs may be tasked with training hundreds of medical professionals, including OB-GYNs, pediatricians, and clinicians with limited trauma or emergency experience, for battlefield or mass casualty medicine in a matter of hours. While training equipment may be maintained at each center, healthcare simulation programs share healthcare simulation instructors and training spaces out of solidarity and professional camaraderie, driven by the urgent, widespread need for rapid readiness. Healthcare simulation professionals may have to travel to other training centers to help prepare soldiers for deployment to multiple trauma zones.
This massive scale demands a mobile, rapidly deployable training system that could adapt to improvised spaces without a compromise in the quality or accuracy of training. A step-by-step process can be followed to provide these rapid pivots that meet the needs of a population.
Step 1: Build a Mobile Simulation Framework
Emergencies require a simulation program that can travel anywhere and start training immediately. Unlike the structured schedule of traditional centers, the system had to be ready for rapid deployment. From the start, consider a deliberate investment in mobile, portable equipment, portable manikins, Portable monitoring simulators, and portable debriefing technology such as cameras and iPads, rather than fixed installations, based on lessons from earlier catastrophes and military operations. This forward-thinking approach allows a healthcare simulation program to respond quickly when facilities become unsafe or unavailable. During these events, informal collaboration between centers, rather than a centralized system, must be emphasized, built on a network of mutual understanding and a shared mission.
- Design training plans assuming constant relocation — deployment in classrooms, hospital corridors, or shelters.
- Assign dedicated logistics roles for equipment transport, setup, and teardown.
- Maintain duplicate sets of essential simulation assets for parallel site operations.
- Create a streamlined operations guide with clear visuals to accelerate deployment.
View the HealthySimulation.com Webinar Time to Go Mobile! Building a Mobile Simulation Lab for Better Patient Outcomes to learn more!
Step 2: Assemble Modular “Pick up and Go ” Kits
The key to speed was the previously prepared modular kits that contained only the essential equipment for each scenario.
- Pre-pack skill-specific kits (bleeding control, airway management, IV access) or create duplicated Trauma kits that include everything that is needed to treat trauma patients.
- Use color-coded containers or stickers for quick identification.
- Include laminated quick guides in every kit for setting up and teardown.
- Favor manual or battery-powered solutions to minimize reliance on power, and always make sure they are fully charged.
- Stockpile duplicates to enable multiple sites to train simultaneously .
Step 3: Rapid Scenario Design and Adaptation
Perfect replication is not always possible to create a realistic environment. Instead, scenarios focused on critical decision-making and teamwork in a battle or other crisis environments, prolonged evacuation, and extended pre-hospital care.
- Build a scenario library with modules easily adapted to any room or environment.
- Prioritize life-saving actions and triage decisions over aesthetic accuracy.
- Use props and simple moulage kits to create psychological immersion quickly.
- Keep simulations short and high-impact to train larger numbers in a limited time.
Step 4: “Train-the-Trainer” Programs
Scaling training required a multiplier effect. We implemented a structured train-the-trainer system to rapidly expand instructor capacity, complemented by a debriefing module kit designed for ease of use. This kit allows both experienced and novice instructors to facilitate structured debriefings with confidence, ensuring consistent messaging and effective learning across all training sessions.
- Create a tiered model: core experts train facilitators, who then train peers.
- Run micro-workshops to cover scenario delivery and rapid debrief techniques.
- Provide facilitator guides to maintain consistent messaging.
- Encourage peer-led mini-debriefings to spread knowledge efficiently.
Step 5: Agile Debriefing Without Video
Frequent movement and improvised spaces means that video playback is not always possible.
Some alternatives to consider are:
- Adopt Plus/Delta or Stop/Start/Continue formats for structure.
- Conduct immediate on-location debriefs to reinforce lessons.
- Limit to 2–3 key takeaways per exercise to prevent overload.
- Use flip charts, portable whiteboards, or even paper for visual emphasis.
Step 6: Logistics and Field Deployment
Efficient logistics are crucial to moving training setups quickly and effectively during a crisis, even without a formal coordination plan between centers. Each site operates independently with their own gear and workflows, while informal collaboration allows all healthcare simulation professionals to share expertise and support where needed.
- Use modular checklists: Clear, scenario-specific lists reduce the chance of missing critical items.
- Standardized packing systems: Consistent methods for organizing gear helped cut setup time dramatically.
- Collaborate informally between centers: Instructors and physical spaces were shared when necessary, strengthening capacity and ensuring training coverage.
View the new HealthySimulation.com Community Pre Hospital Simulation Group to discuss this topic with your Global Healthcare Simulation peers!
Step 7: Precision, Cognitive Load, and Mental Preparedness
Consider when training clinicians under actual stress, many of them may have little or minimal trauma patient experience. This requires a laser focus on clarity and simplicity.
- Deliver “take-to-battle” messages: short, actionable interventions to recall under fire.
- Reduce cognitive load by repetition and simplification.
- Provide frameworks but allow instructors to improvise where needed.
- Focus on decision-making confidence rather than technical perfection.
- Normalize imperfection: “good enough and fast enough” saves lives.
Step 8: Improvisation as a Core Skill
Improvisation is vital, and instructors learned to repurpose available spaces while maintaining high-quality simulation delivery.
- Quickly adapt hallways, rooms, or shelters for training.
- Use common equipment to create realistic casualty zones.
- Keep a mental library of simplified methods to handle shortages.
- Encourage flexibility as a deliberate skill.
Experience demonstrates that simulation can be mobile, scalable, and effective even under extreme pressure. By focusing on core, on-point messages, modular equipment, and collaboration between centers, we built a system that could train medical teams anywhere, anytime, with uncompromising quality.
The transformation of a traditional simulation center into a crisis-ready training network requires a transition from perfectionism to excellence, the ability to embrace adaptability, and build a culture of professional solidarity. With preparation, strong logistics, and flexible training design, simulation becomes a life-saving tool not only for routine practice but in the response to an emergency to save lives impacted by a mass casualty event.
Learn More About How Mobile Simulation Centers Train Learners on the Go!