In graduate medical education, the Accreditation Council for Graduate Medical Education (ACGME) establishes essential standards for residency and fellowship programs across the United States. This HealthySimulation.com article by Rémy Roe, PhD and Simulation Technology Specialist at the Stanford University School of Medicine Center for Immersive and Simulation-based Learning (CISL) explores how healthcare simulation serves as an effective tool for the assessment of the six ACGME core competencies: Patient Care, Medical Knowledge, Practice-Based Learning and Improvement, Interpersonal and Communication Skills, Professionalism, and Systems-Based Practice. Comprehension of these connections helps simulation centers create targeted educational experiences that support residency program accreditation requirements.
The ACGME Core Competencies Framework
The ACGME core competencies provide a comprehensive framework for physician development during residency and fellowship training. These six domains encompass the essential skills and attributes necessary for medical practitioners to deliver high-quality patient care in modern healthcare environments. Each competency addresses specific aspects of physician performance, from clinical knowledge to interpersonal abilities. Together, they form a holistic approach to medical education that extends beyond traditional knowledge acquisition to include professional behaviors, communication skills, and systems thinking.
Residency programs must demonstrate how they teach and assess these competencies to maintain accreditation. Healthcare simulation is a valuable tool for graduate medical education programs that offers a controlled environment for both education and assessment across all six domains.
Patient Care Assessment Through Simulation
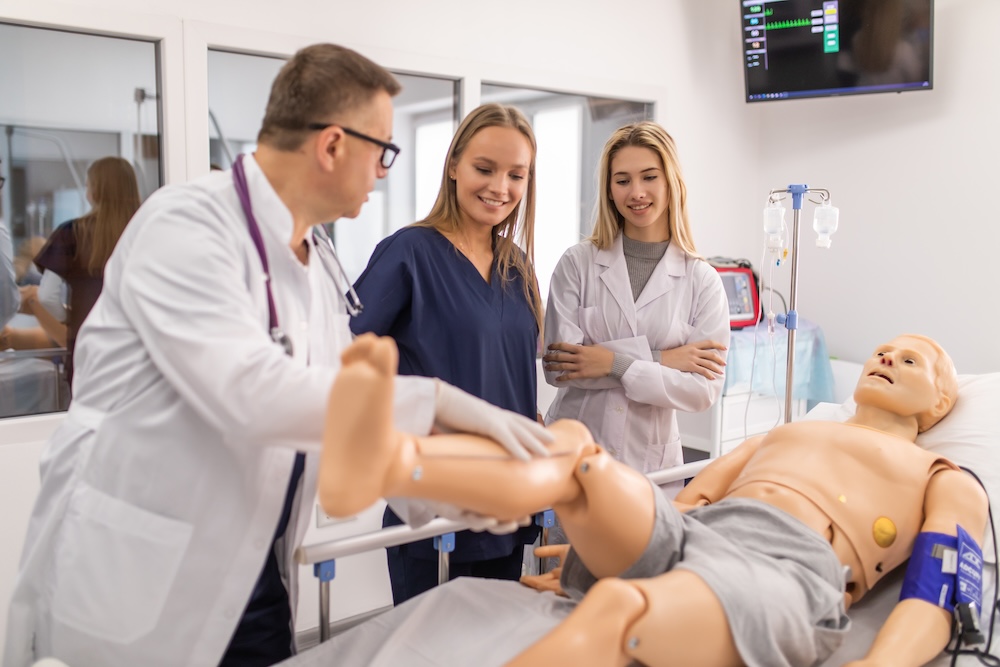
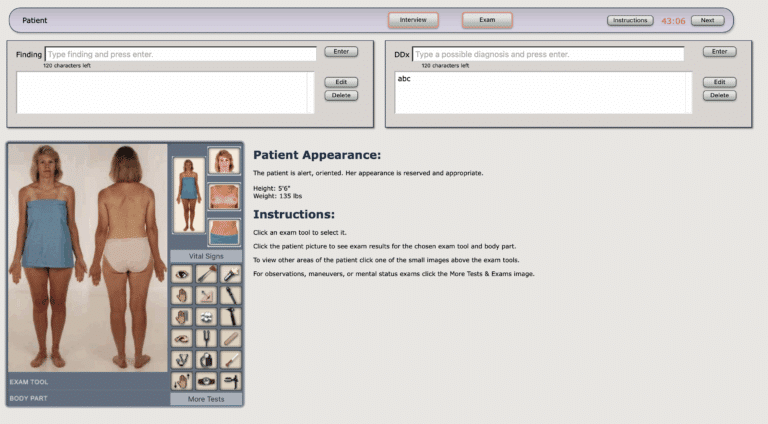
The Patient Care competency focuses on the provision of compassionate, appropriate, and effective care for health promotion, disease prevention, diagnosis, and treatment. Healthcare simulation provides numerous opportunities to assess this fundamental competency. High-fidelity scenarios allow residents to demonstrate clinical skills without risk to actual patients. Evaluators can assess how residents gather information, perform physical examinations, develop diagnostic impressions, and create treatment plans under controlled conditions.
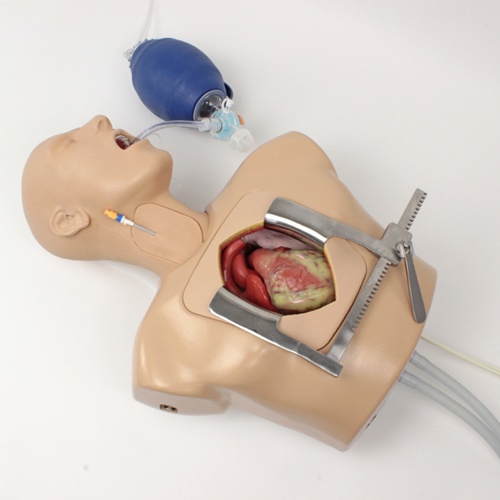
Procedural simulations enable the assessment of technical skills across various specialties. From basic procedures like intravenous line placement to complex surgical techniques, task trainers and virtual reality systems allow objective evaluation of procedural competence. Standardized patient encounters permit evaluation of history-taking approaches, physical examination techniques, and patient education skills. These interactions reveal how residents translate medical knowledge into practical patient care activities.
Medical Knowledge Evaluation
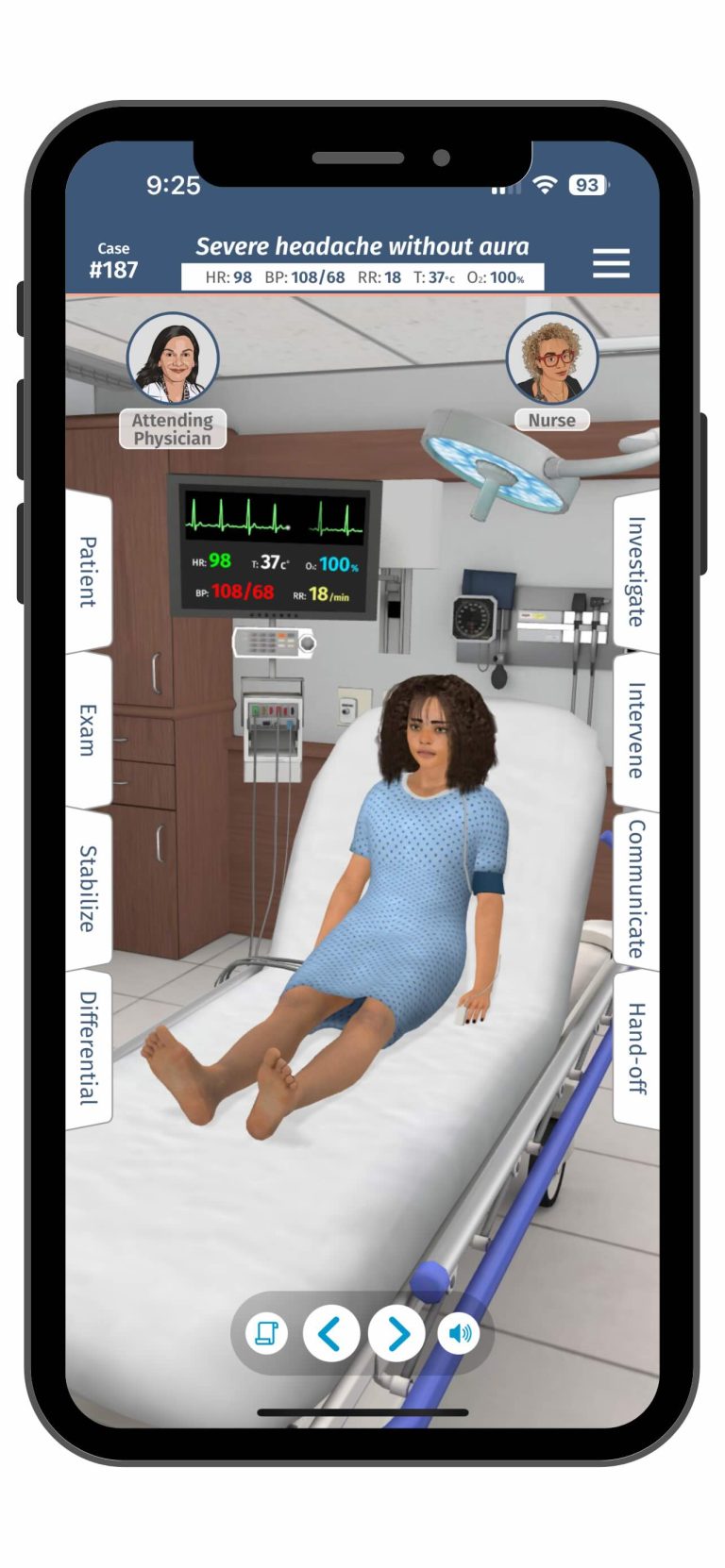
The Medical Knowledge competency encompasses the comprehension of biomedical, clinical, and social-behavioral sciences and their application to patient care. Clinical simulation scenarios can effectively assess this knowledge in action. Case-based simulations challenge residents to apply their medical knowledge to complex clinical situations. These scenarios can target specific conditions or present diagnostic dilemmas that require a comprehensive understanding of disease processes.
Simulation debriefing sessions reveal the depth of resident knowledge through thoughtful questions and discussion. Facilitators can probe the logic behind clinical decisions and, in turn, uncover both strengths and gaps in medical knowledge. Virtual patients and computer-based simulations can track diagnostic pathways and treatment decisions, which creates objective measures of medical knowledge application. These tools allow for standardized assessment across multiple learners.
Practice-Based Learning and Improvement
The Practice-Based Learning and Improvement competency involves investigation and evaluation of care practices, appraisal of evidence, and continuous improvement of patient care based on constant self-evaluation and lifelong learning. Video-recorded simulations allow residents to review their own performance, identify areas for improvement, and develop action plans for skill enhancement. This self-assessment process directly addresses the reflective component of this competency.
Repeated simulation experiences with progressive difficulty permit assessment of improvement over time. Programs can document how residents incorporate feedback from earlier sessions into their subsequent performance. Team-based simulation scenarios can assess how residents contribute to quality improvement discussions and implement changes based on performance data. These activities mirror real-world quality improvement processes.
View the HealthySimulation.com Webinar Unlocking the Potential: Harnessing Clinical Simulation to Drive Competency-Based Education to learn more!
Interpersonal and Communication Skills
The Interpersonal and Communication Skills competency focuses on effective information exchange and collaboration with patients, their families, and health professionals. Clinical simulations provide ideal opportunities to assess these critical skills. For example, standardized patient encounters allow for structured evaluation of communication skills across various clinical contexts. Assessors can observe how residents establish rapport, explain complex medical information, and respond to patient concerns.
Breaking bad news scenarios can also assess residents’ ability to communicate difficult information with empathy and clarity. These emotionally charged simulations reveal communication skills under stress. Finally, team-based resuscitation or crisis management scenarios demonstrate how residents communicate with colleagues during high-stakes situations. Clear communication, closed-loop techniques, and leadership abilities become readily apparent in these environments.
Professionalism Assessment
The Professionalism competency encompasses commitment to professional responsibilities, adherence to ethical principles, and sensitivity to diverse patient populations. Healthcare simulation creates unique opportunities to assess these attributes. Ethical dilemma scenarios challenge residents to demonstrate professional values when faced with complex situations. Their responses reveal adherence to ethical principles and professional standards.
Standardized patients from diverse backgrounds allow assessment of cultural sensitivity and adaptability in clinical encounters. These interactions show how residents modify their approach based on individual patient needs. Interprofessional simulation scenarios demonstrate how residents interact with other healthcare team members. These sessions reveal respect for others’ expertise, collaborative attitudes, and professional boundaries.
View the new HealthySimulation.com Community Medicine Simulation Group to discuss this topic with your Global Healthcare Simulation peers!
Systems-Based Practice Evaluation
The Systems-Based Practice competency involves awareness of and responsiveness to the larger context and system of healthcare. This competency includes the ability to call on system resources to provide optimal care. Clinical simulation scenarios can effectively assess this system’s perspective.
Large-scale disaster simulations or mass casualty exercises assess resident comprehension of healthcare system resources and limitations. These scenarios reveal how residents prioritize care when resources become constrained. Handoff simulations demonstrate the resident’s ability to transition care effectively within healthcare systems. These critical communication events highlight learner comprehension of system continuity.
Finally, Resource allocation scenarios challenge residents to balance individual patient needs with system constraints. These simulations assess awareness of cost, quality, and access considerations in healthcare delivery.
Competency-Based Medical Education Through Simulation
This article, by Rémy Roe, PhD and Simulation Technology Specialist at the Stanford University School of Medicine Center for Immersive and Simulation-based Learning (CISL) has discussed the various ways healthcare simulation can assess the six ACGME core competencies in graduate medical education. Through the creation of targeted clinical simulation experiences, programs can effectively evaluate resident performance across multiple domains simultaneously.
The integration of simulation-based assessment into residency and fellowship programs provides valuable data for both formative and summative evaluation. These assessments help program directors identify areas for curriculum enhancement and document competency achievement for accreditation purposes. As healthcare simulation technology continues to advance, new opportunities for competency assessment will emerge. Virtual reality, augmented reality, and artificial intelligence applications will further enhance the ability of simulation centers to provide an objective, reliable assessment of ACGME core competencies.
The thoughtful application of simulation-based assessment strengthens graduate medical education programs and prepares residents for the complexities of modern healthcare practice. This approach ensures that future physicians develop the comprehensive skillset necessary to provide excellent patient care in an ever-changing healthcare environment.