Healthcare simulation offers the opportunity for learning in a setting that is realistic, founded on experiential learning, and offers the ability to learn from mistakes. One area where healthcare simulation has growth potential is in the area of culture, diversity, and disability. The United States (US) is one of the most diverse countries; cultural geographer Colin Woodward estimates that there are as many as eleven distinctcultural areas in the US based on settlement history. Moreover, disability impacts a significant number of individuals. Per the World Health Organization, 16% of the world’s population lives with some degree of disability, but this figure may be higher in developing nations. Given the diversity of the US and world’s countries (fun fact Uganda is the most diverse nation) and the significant number of individuals with disability, future and current healthcare providers need the skills and knowledge to fully meet the unique needs of the whole-person and provide strong patient / family – centered care delivered well at each and every patient care encounter. This HealthySimulation.com article by Jill Sanko, PhD, APRN, CHSE-A, FSSH, will explore strategies and resources to incorporate culture, diversity, and disability into healthcare simulation education.
Call to Action for Culture, Diversity, and Inclusion in Healthcare Simulation
A recent editorial by Diekmann and Nirula (2024) invited “the broader healthcare simulation community to move beyond the superficial to explore more expansively and deeply these issues” of culture, diversity, and inclusion within medical simulation. Our field has advanced the discussion on considerations and applications of clinical simulation in exploring issues of structural racism and implicit bias, but there continues to be room to do more scholarly / theoretical work and broaden its educational use in the areas of culture, diversity, and disability education.
Recent work has shown that simulation-based education can help to reduce bias and shift perspectives and behaviors. Despite evidence that simulated healthcare has been used to train providers for more than two decades, more work needs to be done as some have argued that on the whole, healthcare simulation-based disability awareness education has not resulted in measurable shifts in attitudes toward those with disability and too often depict disability using the lens of medicalization rather than individual differences. More recent work, however, is shifting this finding and supports the notion that simulation-based education is a promising and viable educational tool for disability awareness. Newer results have shown simulation-based education to be a valuable resource that merits further development and efforts to broaden its use coupled with ongoing longitudinal evaluation via rigorous methods to improve the ability to assess the impacts.
Cultural Awareness Brings Space for Awareness
Use of healthcare simulation to improve cultural awareness has shown more solid outcomes, with significant positive impact on improving cultural awareness, humility, and competence, but even with these positive research results, there is more work to be done. Research gaps exist in evaluating sim scenario effectiveness and integrating cultural humility specifically. A 2023 scoping review offers good recommendations for future work including: ensuring curricula are comprehensive, intentionality about around psychological safety, facilitator education in how to run prebrief sessions that make learning objectives and learner expectations clear, development and delivery of highly structured debriefs, and direct observation of learners, along with formative feedback, to promote self-reflective practices.
View the HealthySimulation.com Webinar Designing Medical Simulation Scenarios with AI and ChatGPT to learn more!
Healthcare Simulation Modalities for DEI
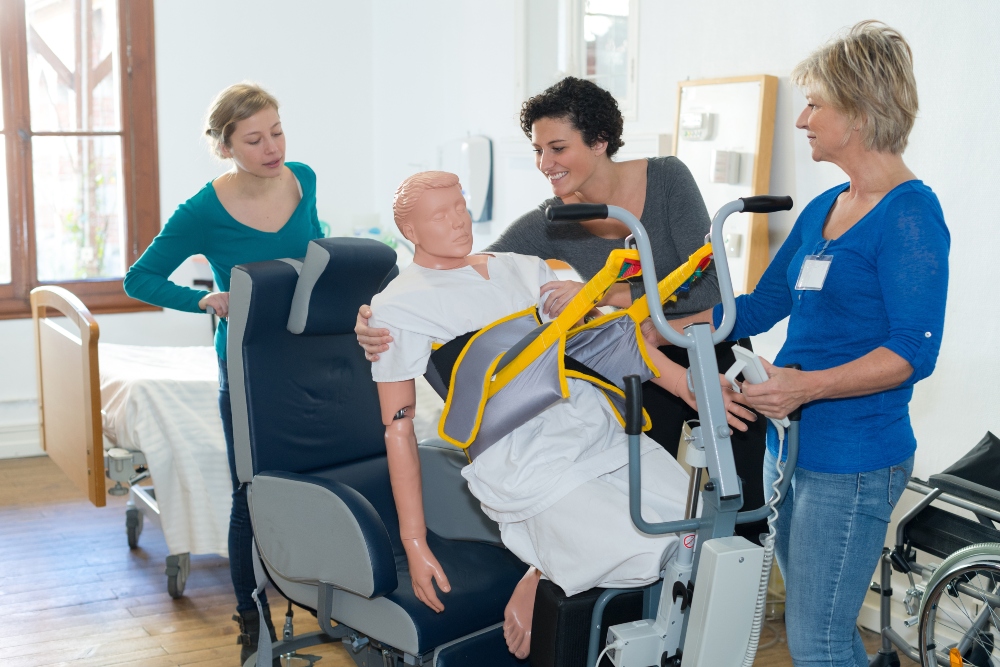
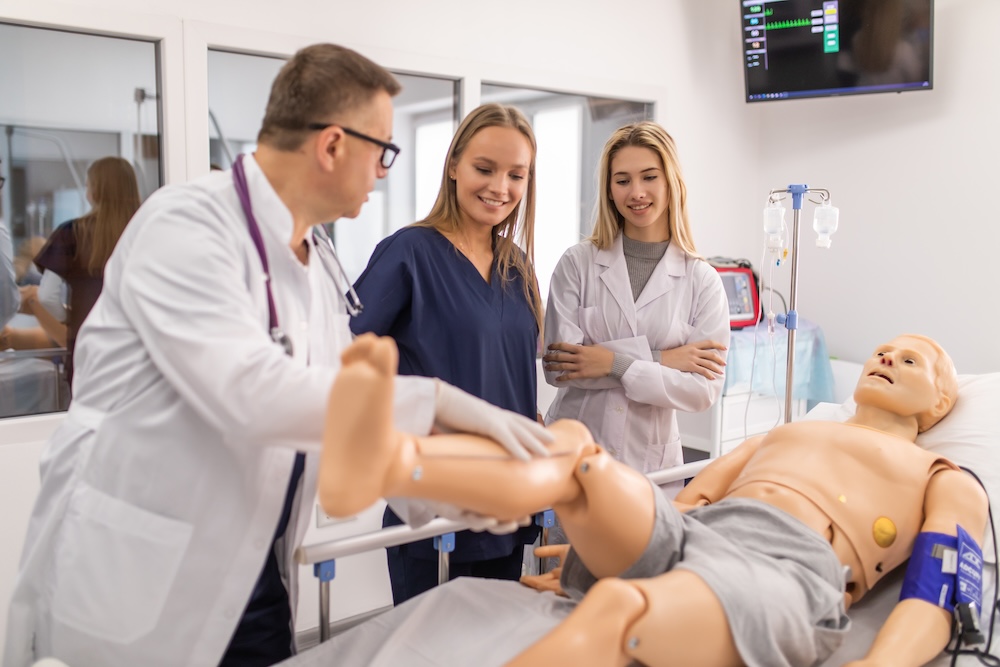
There are many formats of healthcare simulation that can improve knowledge, skills, and awareness of culture, diversity and disability including mannikin-based, standardized / simulated patient/ actor-based, role-play, table-top / games, and virtual reality. The use of simulated participants / standardized actors appears to be the most widely employed type used in this space. Role-play is also commonly used.
Each format has pros and cons to consider, but regardless of the type employed care needs to be taken to carefully vet for appropriate depictions of each topic presented to mitigate negative lessons. If a team is creating a scenario / activity, care needs to be taken to solicit the opinions of those with the condition or who are a part of the cultural group as well as those who work with them. Collaboration is key in creating strong scenarios that fully offer the opportunity to learn about culture, diversity, and disability. By engaging a 360 comprehensive assessment of each scenario / activity prior to use, educators can be assured that the depictions are true to how both in-group and out-group members experience reality and perceive the world. A key consideration when using simulated participants / standardized actors is to use members of the particular target group. Great care also needs to be taken when using role play to avoid negative depictions of groups inadvertently.
The use of individuals with disabilities to depict the patient has been done with some level of success for at least a decade, and should be considered as a viable method for clinical simulation-based disability education. The National League of Nursing offers a guide for incorporating individuals with disabilities into simulation scenarios / curricula. In addition the Hastings Center for Bioethics offers a nice guide for educators on anti-ableist education. A 2025 integrative review noted the importance of integrating disability into SBE to improve knowledge and understanding, communication confidence, empathy, and enlightened attitudes, but emphasized the need for large well-designed studies to measure its effectiveness.
Culture-Focused Healthcare Scenarios
Culture-focused scenarios can depict various situations that include language barriers, religious practices, death and dying practices, dietary needs, and illness beliefs. Culture-centric medical simulation scenarios can portray a variety of situations. These include, but are not limited to: language barriers, religious and death/dying customs, dietary requirements, and beliefs surrounding illness.. The University of Minnesota Center for Advanced Research on Language Acquisition has a nice resource that lists a number of healthcare simulations and games to expand awareness, knowledge, and skills related to culture and cultural practices. In addition, the use of standardized patient / simulated patient / actor-based healthcare simulation that uses members of the group you aim to educate about offers the most robust learning opportunity for learning about and with the other. The goals of these clinical simulation encounters are to increase awareness and promote cultural humility. While many aim for cultural competence as an end goal, this can be a foolish errand, as only those who are members of a particular group can truly become culturally competent.
View the new HealthySimulation.com Community Scenario Design Group to discuss this topic with your Global Healthcare Simulation peers!
Healthcare simulation scenarios can create immersive experiences that allow participants to encounter diverse perspectives and values in a safe, controlled environment; this relative safety can foster cultural and diversity awareness and sensitivity that cannot be produced in a classroom when done with care. The ability to learn about differences and how to care for a diverse patient population in an environment where mistakes are allowed, free from the fear of errors or the possibility of causing offense to others, is a major advantage of SBE.
Thiswork is not easy, which comes with risk and vulnerability, but there is a greater risk of not expanding healthcare simulation as a tool for this purpose. If we do not wield the power of simulation-based education to teach much needed diverse perspectives and considerations in the care of all peoples, we will fail to have the healthcare team and system which will most effectively care for the infirm and vulnerable, risking being forever doomed to repeat a cycle of “almost care” where we might heal, but fall short of whole-person / full care. There is value in diversity. There is more value in meeting the diverse needs of all patients. As a community, we should heed the call for further expansion of simulation in the quest to fulfill the promise of health equity.
Tackling this work is challenging, fraught with risk, and vulnerability. However, neglecting to broaden the healthcare simulation’s scope for this purpose carries a far greater danger. Should we fail to harness healthcare simulation-based education to impart crucial diverse viewpoints and considerations in patient care, we will lack a healthcare workforce and system capable of effective care for the ill and vulnerable. Consequently, we risk perpetuating a cycle of insufficient care, where physical healing occurs but holistic, comprehensive care falls short. Diversity holds value, but addressing the varied needs of all patients holds even greater value. As a community, we must answer the call to further expand medical simulation in pursuit of achieving health equity.
Learn More About DEI Education in Simulation!
Resources
- French, S. (1992). Simulation Exercises in Disability Awareness Training: A Critique. Disability, Handicap & Society, 7(3), 257–266. https://doi.org/10.1080/02674649266780261
- Grégoire,. B., Attoe, Chris; Marshall-Tate, K.,; Riches, S,.; Wheildon, J., ; et al. Simulation training to support healthcare professionals to meet the health needs of people with intellectual disabilities. Advances in Mental Health and Intellectual Disabilities; 10(5), 284-292. DOI:10.1108/AMHID-08-2016-0018
- Hastings Center for Bioethics Anti-Ableist Medical Education: Meeting the Challenges
- National League of Nursing guide: Guide for Integrating Standardized Patients with Disabilities in Nursing Curriculum
- University of MN CARLA resource for cultural simulation and games.
References
- Carman, Luke MS; Lim, Fidelindo DNP,. Simulation-Based Learning About Care of People With Disabilities: An Integrative Review. Nurse Educator 50(3):p E146-E151, May/June 2025. | DOI: 10.1097/NNE.0000000000001788
- Dahlen, B., McGraw, R., and Vora, S. (2024). Evaluation of simulation-based intervention for implicit bias mitigation: A response to systemic racism, Clinical Simulation in Nursing, 95, https://doi.org/10.1016/j.ecns.2024.101596.
- Daya, Sneha MD; Illangasekare, Tushani MD; Tahir, Peggy MLIS, MA; Bochatay, Naike PhD; Essakow, Jenna MD; Ju, Mindy MD, MAEd; van Schaik, Sandrijn MD, PhD. Using Simulation to Teach Learners in Health Care Behavioral Skills Related to Diversity, Equity, and Inclusion: A Scoping Review. Simulation in Healthcare: The Journal of the Society for Simulation in Healthcare 18(5):p 312-320, October 2023. | DOI: 10.1097/SIH.0000000000000690
- Dieckmann, P., Nirula, L. Moving towards deep equity, diversity, inclusivity and accessibility in simulation: a call to explore the promises and perils. Adv Simul9, 6 (2024). https://doi.org/10.1186/s41077-024-00278-3
- Thomas B, Courtenay K, Hassiotis A, Strydom A, Rantell K. Standardised patients with intellectual disabilities in training tomorrow’s doctors. Psychiatr Bull (2014). 2014 Jun;38(3):132-6. doi: 10.1192/pb.bp.113.043547. PMID: 25237524; PMCID: PMC4115377.