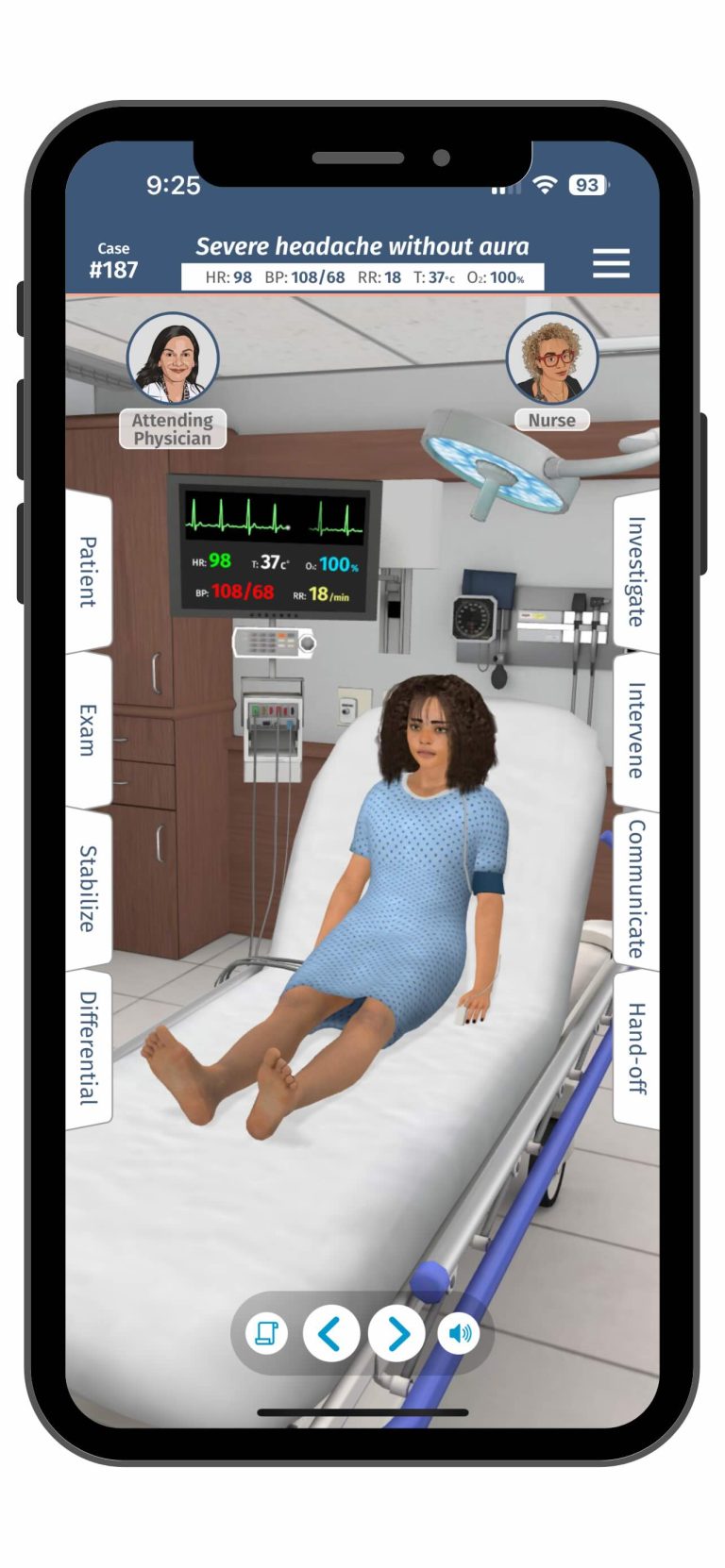
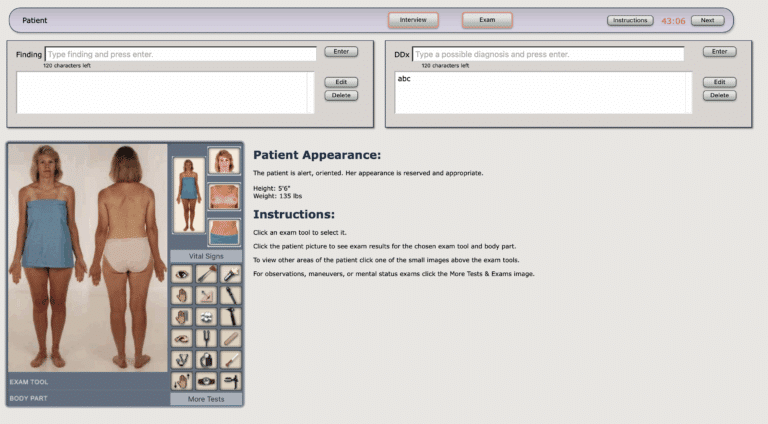
Medical simulation training has become an essential pillar for the healthcare system. Clinical simulation not only provides knowledge but also prepares for readiness of healthcare professionals before exposure to real-life scenarios. Medical simulation learning has replaced our orthodox learning method, which relied more on real patient exposure and textbook reading. Medical simulation learning is a new emerging learning method, so close monitoring and routine assessment should be done to check the effectiveness. To ensure quality healthcare simulation is conducted, there must be a process for quality assurance. This HealthySimulation.com article by Dr. Bhavesh Patel will explore quality assurance frameworks and strategies for effective medical simulation training.
What is Quality Assurance?
Patient safety is the uppermost priority in the healthcare system. If trainees are undertrained, they cannot manage real scenarios effectively, and this can risk patients’ lives. Quality assurance ensures the standardization of the learning process, in which all trainees should receive equal exposure while training. At the end of the training, all trainees should achieve adequate skills to perform in real-world situations. Even after adequate training with simulation, trainees can get confused by the complexity of real scenarios. If trainees have completed training with good adherence to protocols and achieved an adequate level of skills,this will be reflected by either the patients’ outcome or improvement in critical healthcare data.
Multiple quality improvement frameworks are frequently used in healthcare and healthcare simulation. These are LEAN, Six Sigma, and PDSA. The frameworks discussed in this article are PDSA and Six Sigma.
PDSA: Plan, Do, Study, Act
PDSA is a rapid cycle quality improvement tool which works on the Plan-Do-Study-Act method. This can be used in new simulation technology before integrating them into a curriculum. This also can be used to improve debriefing structure, team performance and checklist usability. Six Sigma focuses on reducing variability and improving reliability of processes through data-driven analysis.
Six Sigma Data-driven Methodology for Improving Processes
The DMAIC structure is used in the Six Sigma framework for the core structure improvement cycle. DMAIC means Define – Measure – Analyse – Improve – Control. Quality and performance of simulated fidelity are linked to successful training. With DMAIC, variability and errors of simulated fidelity can be reduced. This can identify the issue with fidelity, the current level of effectiveness of fidelity on performance, and the root cause of variability. With this data, DMAIC can help to implement the target solutions and maintain the improvement over time.
Key Parameters of Quality Check
Key components can serve as a checklist to ensure the adequate delivery of debriefing.
Pre-training assessment and preparedness: Before the beginning of the training, all trainees should go through a basic knowledge assessment regarding the related topic through a pretest. The pretest score can be compared to the post-test score to check improvement in knowledge.
Quality of debrief and faculty competency: Debriefing is the most important tool in medication simulation training. Debriefing depends on the facilitator’s experience and knowledge about the given topic. Good debriefing can encourage trainees to learn new skills. Poor debriefing can create confusion among trainees and can eventually bring negative outcomes. Quality of debriefing is assessed by the DASH score. This is the debriefing assessment for simulation in healthcare. This has seven components:
- Create an engaging environment among trainees.
- Maintain respect and trust between trainees and the facilitator.
- Structure the logical debriefing for clear insight.
- provoke discussion during debriefing.
- Identify potential performance gaps.
- Helps the trainees to achieve good performance.
- Demonstrate effective communication.
View the HealthySimulation.com Webinar Turn Right Here: Driving Healthcare Quality Improvements to learn more!
Scoring and Performance Assessment of Trainees: Different types of score systems can be used to assess the performance of trainees. Ottawa Global Rating Scales and OSATS (Objective Structured Assessment of Technical Skills) are two scoring methods. Ottawa Scales is a non-technical skill-based scoring system. This can assess leadership, communication, teamwork, or decision-making steps taken by trainees. This is used in scenarios where a multidisciplinary approach is necessary, such as the triage of patients during mass emergencies. OSATS is used for technical skills. Each step in a skill is given a score. In neonatal resuscitation, all the important steps are considered in checklists. Each correct step is marked as a score of 1. At the end of the procedure, a final score is assigned based on the trainee’s performance. New AI technology, with a combination of high-fidelity simulated devices, can generate automated simulated data and scoring. Repeated training, along with this score improvement, can give an idea about successful skill achievement.
Learners’ Outcome and Impact: The immediate outcome can be assessed by comparing pre-test and post-test scores or skill-based scoring performance. Long-term outcome is measured with trainees’ performance on a real task with real patients and their retention of knowledge during the procedure or skill. System outcomes are considered positive if there is an improvement in adverse events or a reduction in the mortality rate over time.
Learners’ Feedback: Learners’ feedback can give an idea about the whole simulation training, from briefing to performance. Whether training was stressful or safe, a learning environment was created successfully with or without any pressure, and whether they had achieved enough confidence to perform skills on real patients or not. All this feedback can help to improve the training.
View the new HealthySimulation.com Community Administrators Group to discuss this topic with your Global Healthcare Simulation peers!
Need for an Accreditation Body: There should be a body that can conduct all these quality assurances and provide accreditation to simulation labs. In the United States, the Society for Simulation in Healthcare (SSH) performs this duty. The SSH accreditation process has five parameters: standard, education, assessment, research, and system integration with healthcare. This ensures the reliability and effectiveness of simulation training. INACSL is an International Nursing Association for Clinical Simulation and Learning that focuses on training paramedical health workers with effective simulation training. ASPiH accreditation provides quality assurance for both individuals and institutions.
Research and Development: Research and development are essential for the progress and effectiveness of simulation learning. These can make medical simulation more dynamic and accessible. Research on how to integrate artificial intelligence or augmented reality with high-fidelity simulators can revolutionize all of medical simulation learning in the future. There are several bodies that actively participate in research and development of training programs for medical simulation training.
The Healthcare Simulationist Code of Ethics: The code of ethics in medical simulation was introduced to bring safe, respectful, and effective learning with patients safely and confidentially. There should be maintenance of professionals’ integrity and honesty. respect for participants, psychological safety, transparency, and competency from educators. Where learners have responsibilities like engagement and respect, professionalism, and honesty in reflections. Institutions also have responsibilities like simulation governance charter, non-punitive learning culture, privacy and security, faculty credentials, and continuous medical education.
Legal Aspects: Simulated training is conducted with video and audio recordings. Consent must be obtained from all trainees before they are enrolled in the learning program. Trainees’ data should not be misused for any other purpose. Some scenarios can reparent vulnerable populations, like child abuse or psychiatric illness. Such scenarios should be portrayed with respect and sensitivity.
There are multiple dimensions to check the quality of medical simulation learning. Regular scrutiny and maintaining training standards can bring positive outcomes with medication simulation learning.
Learn About the IHI Quality Improvement Essentials Toolkit Helps Optimize Outcomes!
References:
- Rider A, Schertzer K. Quality Improvement in Medical Simulation. [Updated 2023 Jul 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing
- Furman, Gail & Smee, Sydney & Wilson, Crystal. (2010). Quality Assurance Best Practices for Simulation-Based Examinations. Simulation in Healthcare: Journal of the Society for Simulation in Healthcare.
- Ekelund, K., O’Regan, S., Dieckmann, P., et al. Evaluation of the simulation-based training quality assurance tool (SBT-QA10) as a measure of learners’ perceptions during the action phase of simulation.