The Association of Standardized Patient Educators (ASPE) is a global organization focused on human simulation via Standardized Patients, aka Simulated Patients. Headquartered in Altamonte Springs, Fla., the organization serves as a virtual community for connection to the field of medical simulation. Designed with member convenience in mind, ASPE is responsive and easily accessible from a computer, phone or personal device.
Through these devices, the Association of Standardized Patient Educators includes social networking support and simple tools for connecting colleagues throughout the growing simulation community. Guiding these efforts, the mission of the ASPE is to advance standardized patient-based pedagogies, assessments, research, and scholarships.
Note: In the United States these specialized actors are called Standardized Patients, but elsewhere in the world these educational professionals are also referred to as Simulated Patients.
ASPE Mission and Purpose
As the international organization of simulation educators, the Association of Standardized Patient Educators is also dedicated to promoting best practices in the application of SP methodology for education, assessment and research. The organization’s added purpose includes fostering the dissemination of research and scholarship in the field of SP methodology, and working to advance the professional knowledge and skills of its members. APSE actively engages their members, educators, and learners to ensure social justice and to embrace inclusivity.
ASPE’s Vision Statement is transforming professional performance through the power of human interaction. ASPE members serve as a great resource and are always ready to help others with SP training, curriculum and program development and center creation. Encouraged to share their expertise and experience regarding anything related to SP methodology, members all around the world provide strength and insight to the association.
Core Values and Strategic Pillars
The strategic pillars are built upon the mission statement, purpose, vision, and core values. The core values are:
- Safety
- Quality
- Professionalism
- Accountability
- Collaboration
The Strategic Pillars are:
- Excellence in Standardized Patient Methodology, Education, Curriculum, and Standards of Best Practice
- Research
- Advance Members and Affiliates
- Vitality and Sustainability
Equity, Diversity, and Inclusion Statement
ASPE is committed to equity, diversity and inclusion. This is demonstrated through open dialogue forums around issues of racial injustice. ASPE advocates and educates regarding EDI at their annual conference and webinars.
In combination with this widespread membership, ASPE’s strength is derived from participating association committees. ASPE membership allows for participation in ASPE’s working committees, as well as the opportunity for election to the ASPE Board of Directors. Participation in committees affords members the opportunity to develop leadership skills, increase professional growth, and to influence the development and direction of the field of simulation in healthcare.
A board of directors helps further govern the Association of Standardized Patient Educators, while ensuring that standards and best practices are followed. Board members are required to attend a monthly, one to two-hour board of director‘s call, travel to and participate in two face-to-face retreats per year (after IMSH and before ASPE Annual) and complete additional outside work on projects that benefit members.
They are also required to be a current ASPE member at the time of nomination and through Board service. The vice president for operations has to attend two additional executive committee meeting calls each month as well.
ASPE further encourages the advancement of SP-based education through special interest groups (SIGs). The SIGs work to strengthen relationships, awareness, knowledge and skills specific to a particular aspect of SP practice. The Educational Content Committee is home to ASPE’s five SIGs: SPs beyond healthcare, hybrid simulation, interprofessional education, Gynecologic Teaching Associate (GTA)/Male Urogenital Teaching Associate (MUTA) and social justice.
Standardized Patient and ASPE History
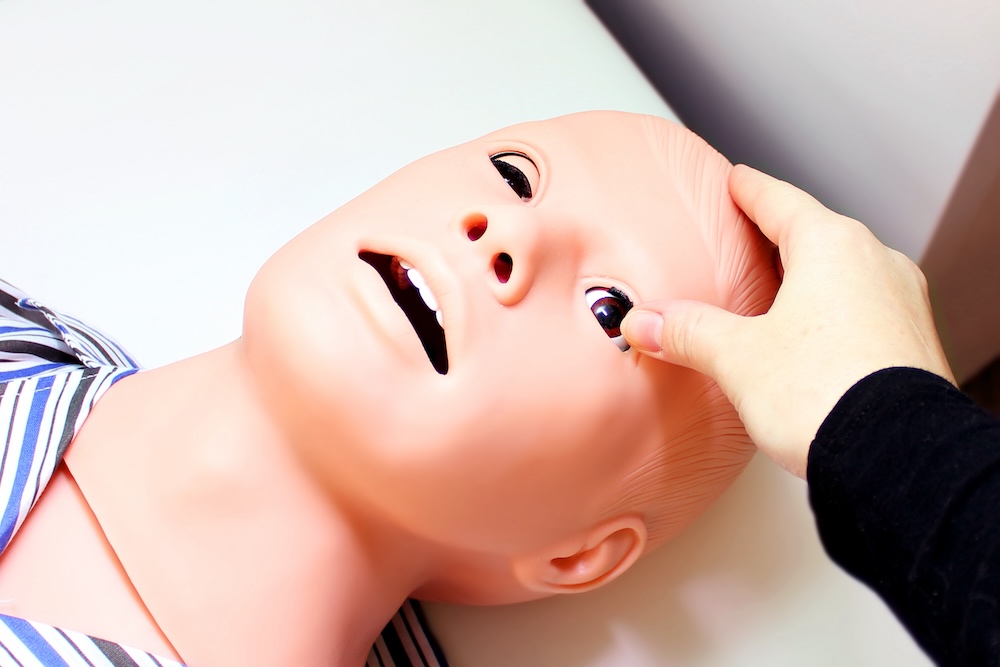
According to the Association of Standardized Patient Educators, when performing simulation, the SP presents the Gestalt of the patient being simulated; not just the history. Rather, the SP presents the body language, the physical findings and the emotional and personality characteristics.
The ASPE shares on the association website that in 1963 a neurologist by the name of Howard Barrows discovered that a lay person could be trained to simulate illness and give feedback to medical students about their history and communication skills. He called this person a simulated patient (SP) and defined the term as “a person who has been carefully coached to simulate an actual patient so accurately that the simulation cannot be detected by a skilled clinician.
Since Barrows’ discovery, the use of the Simulated Patient began to grow in healthcare education. Educators found that Simulated Patients offered not only a variety of teaching opportunities for learners, but also opportunities for testing student performance. Out of this testing environment grew the official term “Standardized Patient” or “SP.”
As simulation and the Simulated Standardized Patient mythology continued to grow, educators felt a need to develop an organization that could foster the growth of the Standardized Patient profession that was creating and supporting this new methodology. As a result, the Association of Standardized Patient Educators was formed in 2001.
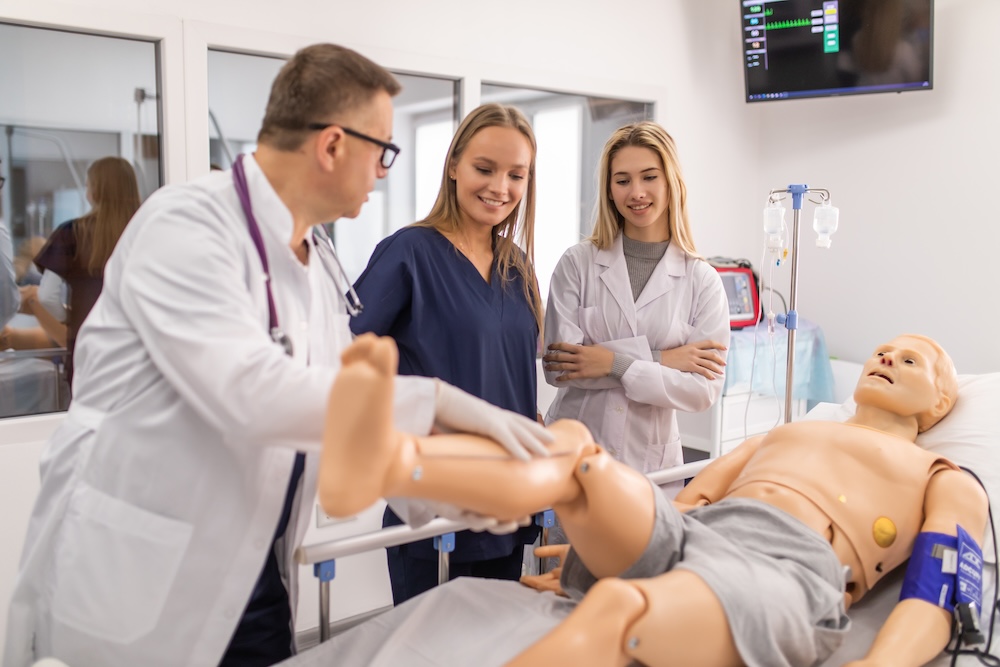
Since then, the organization’s membership has grown along with the concept of the Standardized Patient itself. The expanding use of SPs has widened into many fields including dentistry, pharmacy, veterinary medicine and allied health professions. Over the last two decades, three healthcare simulation modalities have become intertwined – scenarios may now include SPs, task trainers and/or manikins; commonly known as “hybrid” simulations.
Development of ASPE Simulation Standards and GTA / MUTA Standards of Best Practice
Association of Standardized Patient Educators (ASPE) Standards of Best Practice (SOBP) were developed for those working with clinical human role players who interact with healthcare learners in a wide range of experiential learning and assessment contexts. The ASPE SOBP are intended to be used in conjunction with the International Nursing Association for Clinical Simulation and Learning (INACSL) Healthcare Simulation Standards, which address broader simulation practices. These standards are a foundation to guide the practice and management of Standardized Patient Programs for educators who use this methodology in clinical simulation.
The ASPE SOBP were developed by a consensus opinion of experts in the field of SP methodology. The ASPE Board of Directors collaborated with the ASPE Standards of Practice Committee to determine the best practices. A modified Delphi process was implemented to identify the main domains, the principles of the domains, and the practices to achieve the principles. Drafts with revisions of global SP educators occurred in three rounds. The ASPE SOBP results from a team of reviewers and final revisions.
The ASPE Standards of Best Practice defined standardized patients as the terms standardized patient and simulated patient (SP) are often used interchangeably and refer to a person trained to portray a patient in realistic and repeatable ways. SPs interact with learners in experiential education and assessment contexts. Learners, depending on the context, are variously described as students, trainees, participants, examinees, or candidates. SPs can also provide feedback on learner performance from the perspective of the person they portray, which is unique to working with SPs. SP-based education has grown in size and scope of practice to include many different roles. For this reason, the term simulated participant is being used as a more inclusive term to refer to all human role players in any simulation context.
Overall, the context in which Standardized Patients are working determines the degree of repeatability or standardization (consistency and accuracy) of their behavior, both within an individual SP’s performance and between SPs portraying the same role. This behavior can be seen as part of a continuum, according to ASPE. On one end of the continuum, in high-stakes assessment, SPs may be trained to behave in a highly repeatable or standardized manner in order to give each learner a fair and equal chance and are often referred to as standardized patients.
HealthySimulation.com Articles on ASPE Standards: